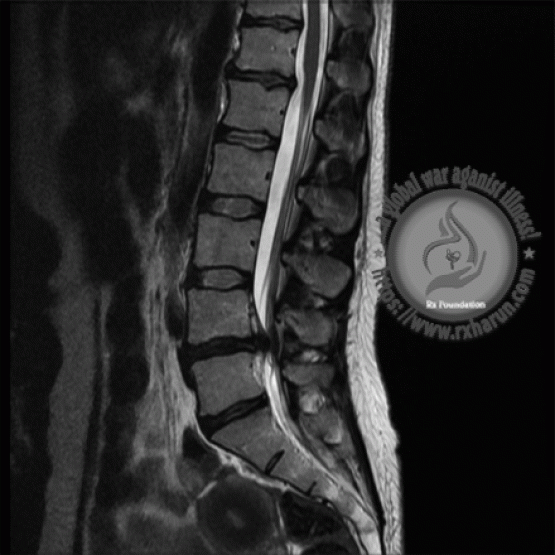
Focal anterior displacement of the thoracic spinal cord on magnetic resonance imaging (MRI) is typically seen in patients with intradural arachnoid cysts or spinal cord herniation. Posterior intradural arachnoid cysts displace and compress the spinal cord by mass effect, whereas spinal cord herniation is a displacement of the spinal cord through a dural defect secondary to a traumatic, postoperative, or idiopathic etiology (rx). Spinal cord herniation has been reported with increasing frequency in recent years, and it is an important differential diagnosis to consider with suspected intradural arachnoid cysts (rx). Once a dural defect has occurred, cerebrospinal fluid (CSF) pulsation may push the cord through the defect, resulting in progressive myelopathy (rx, rx).
Causes Of Posterior Displacement of C5 Vertebra
A Posterior Displacement disc can be caused by many degenerative spinal conditions or an injury. Below are the most common causes of a collapsed disc.
- Aging – Just like every other degenerative spine condition, the natural process of aging is the most common cause for the development of a posterior displacement of the disc. Over time, the discs lose water content making them brittle and less flexible. They’re meant to absorb the shock, acting like cushions for the spine, but they tend to lose their elasticity over time which increases their overall vulnerability. When this happens, the natural wear and tear from day-to-day activities can make it vulnerable to tears and bulging. Eventually, this can lead to diminished height or collapsed disc conditions.
- Weight – Another cause for a posterior displacement of disc condition is overweight problems. Our spine is primarily responsible for the support of our upper body weight. A heavier weight can increase the axial load exposed on the spine. As they are already more susceptible to damage with time, overweight increases the likelihood for the disc to collapse or to flatten out. This causes it to lose its normal shape, which can lead to different symptoms.
- High Impact Sports – Although aging is the most common cause of a posterior displacement of disc condition, participating in high-impact sports can also expose the spine to forceful blows that could potentially lead to a posterior displacement of disc condition. Certain sports can also increase the axial load placed on the spine such as the impact of high-impact sports or repetitive motions such as twisting and swinging.
- Spinal Arthritis – Also known as osteoarthritis, this degenerative condition of the spine is due to aging. Researchers are also learning that some may have a genetic predisposition to spinal arthritis. As the joint structure and function are worn away, the spinal discs, posterior displacement of the disc may collapse causing the facet joints to rub together.
- Degenerative Disc Disease – As spinal discs become weaker and lose water content, this can cause the disc to collapse and posterior displacement of the disc loses height, greatly decreasing the space between vertebra posterior displacement of the disc.
- Herniated Disc – When the interior portion of the spinal disc ruptures the outer portion of the disc, this can cause nerve pain and cause the disc to fully collapse, posterior displacement of the disc.
- Sudden Injury – A serious injury caused by an auto accident, sports injury, or another type of serious injury can immediately cause a disc to collapse where there were previously no symptoms.
- Piriformis syndrome – This develops when the piriformis muscle, a small muscle that lies deep in the buttocks, becomes tight or spasms, which can put pressure on and irritate the sciatic nerve & cause collapsed disc.
- Spinal stenosis – This condition results from the narrowing of the spinal canal with pressure on the nerves. It may lead to posterior displacement of the disc.
- Spondylolisthesis – This is a slippage of one vertebra so that it is out of line with the one above it, narrowing the opening through which the nerve exits with posterior displacement of the disc.
- Cauda equina syndrome – A rare but serious condition that affects the nerves in the lower part of the spinal cord; it requires immediate medical attention. Cauda equina syndrome may permanently damage the nervous system and even lead to paralysis.
- Bony growths (osteophytes) – Osteophytes are bony lumps (bone spurs) that grow on the bones of the spine or around the joints. They often form next to joints affected by osteoarthritis, a condition that causes joints to become painful and stiff.

- Bone spurs – are bony outgrowths on the edges of joints. Bone spurs form where cartilage is worn away (for example in arthritis) and bone is rubbing on bone. In an effort to protect the body, new bone forms on the edge of joints. This is called a bone spur, posterior displacement of the disc. Bone spurs are not painful in themselves, but unfortunately, the bone spurs can rub on nearby bones or nerves, causing problems. In the spine, bone spurs can intrude into space normally reserved for the nerves, thus causing sciatica.
- Sudden injury or accident – Some unexpected traumatic events, such as a car accident, can lead to sciatica. Injuries sustained and new scar tissue can place stress on the sciatic nerve, with posterior displacement of the disc.
- Pregnancy – During pregnancy, pain in the back of the thighs spurred by shifts in the pelvic region can be misdiagnosed as sciatica. However, there are situations in which the sciatic nerve is actually being pressed as a result of these changes. Speak to your doctor if you think you are suffering from sciatica or pelvic groin pain.
- Tumors – within the spine may compress the root of the sciatic nerve.
Symptoms of Posterior Displacement of C5 Vertebra
The following symptoms of a posterior displacement
- Joints that ache during, or after activity
- Back pain and stiffness
- Swelling and warmth
- Pain in the neck, back, low back, arms, or legs for a posterior displacement
- Inability to bend or rotate the neck or back
- Numbness or tingling in the neck, shoulders, arms, hands, hips, legs, or feet for a posterior displacement
- Weakness in the arms or legs for posterior displacement
- Limping when walking
- Increased pain when coughing, sneezing, reaching, or sitting during posterior displacement
- Inability to stand up straight; being “stuck” in a position, such as stooped forward or leaning to the side
- Difficulty getting up from a chair
- Inability to remain in 1 position for a long period of time, such as sitting or standing, due to pain
- Pain that is worse in the morning in posterior displacement
- This is a sharp, often shooting pain that extends from the buttock down the back of one leg. It is caused by pressure on the spinal nerve.
- Numbness or a tingling sensation in the leg and/or foot for a posterior displacement
- Weakness in the leg and/or foot
- Loss of bladder or bowel control. This is extremely rare and may indicate a more serious problem called cauda equina syndrome. This condition is caused by the spinal nerve roots being compressed.
- A feeling of the bones rubbing against one another, especially in the neck, back, and knees for posterior displacement
- Pain/tenderness in the back, hip, knee, or hands that are getting gradually worse over time
- Pain in the back that may radiate to the legs
- Tingling or numbness in the back or extremities
- Mobility or functional issues in the back
- Bladder or bowel control issues
Diagnosis Of Posterior Displacement of C5 Vertebra
History
Your doctor may ask about medical history in which you answer questions about your health, symptoms, and activity. Previous disease condition, fracture, lifestyle, geographical location, food habit, and acute and chronic disease, drug addictions, occupation of the patient for posterior displacement. In the lumbar spine, a herniated disc, and posterior displacement can present with symptoms including sensory and motor abnormalities limited to a specific myotome. History in these patients should include chief complaints, the onset of symptoms, where the pain starts and radiates. History should include if there is any past treatment history.
Pain history for the collapsed disc is-
- Duration – How long the pain is present?
- Onset – How did it start?
- Progress – What happened afterward?
- Site – Where do you feel the pain, point it out with a single finger?
- Character – What is the nature of pain? Is it throbbing, pricking, or burning type of pain?
- The intensity of pain – What is the severity of pain at present, at rest, and during activity? How severe was the worst pain you experienced?
- Temporal factors – Continuous or intermittent, diurnal variation.
- Is the pain continuous or intermittent?
- If intermittent, how long does each episode last?
- If intermittent, is it colicky in nature?
- Is there any relation between the severity of pain and the time of day?
- Is there any sleep disturbance due to pain?
- Aggravating factors.
- Is it aggravated by activity? Suggestive of mechanical pain.
- Is it aggravated when getting up in the morning? If yes, how long does the increased pain last? Morning stiffness is present if the pain lasts for more than one hour. Morning stiffness is suggestive of inflammatory spondyloarthropathy.
- Is it aggravated by walking? Suggestive of vascular or neurogenic claudication.
- Is it aggravated by standing? Suggestive of neurogenic claudication.
- Relieving factors.
- Is it relieved by activity? Suggestive of inflammatory spondyloarthropathy.
- Is it relieved by rest? Suggestive of mechanical pain.
- If aggravated by walking, is it relieved by standing? Suggestive of vascular claudication.
- If aggravated by standing and walking, is it relieved by sitting down or stooping forwards? Suggestive of neurogenic claudication.
-
Manual palpation Test
- Palpation was conducted on the left side-lying position with pressure applied only to the onset of pain (P1).
- The presence of generalized hyperalgesia made it difficult to establish a comparable finding day.
Self-administered, self-reported history questionnaire to diagnose collapsed disc and its clinical subtypes
| Q1 | Numbness and/or pain in the thighs down to the calves and shins. |
| Q2 | Numbness and/or pain increase in intensity after walking for a while, but are relieved by taking a rest. |
| Q3 | Standing for a while brings on numbness and/or pain in the thighs down to the calves and shins. |
| Q4 | Numbness and/or pain are reduced by bending forward. |
| Key questions for diagnosis of cauda equina symptoms: | |
| Q5 | Numbness is present in both legs. |
| Q6 | Numbness is present in the soles of both feet |
| Q7 | Numbness arises around the buttocks. |
| Q8 | Numbness is present, but the pain is absent. |
| Q) | A burning sensation arises around the buttocks. |
| Q10 | Walking nearly causes urination. |
Physical exam
A physical exam to assess your strength – reflexes, sensation, stability, alignment, and motion.
A careful neurological examination can help in localizing the level of the compression. Sensory loss, weakness, pain location, and reflex loss are associated with posterior displacement.
- L1 Nerve – pain and sensory loss are common in the inguinal region. Hip flexion weakness is rare, and no stretch reflex is affected.
-
L2-L3-L4 Nerves – back pain radiating into the anterior thigh and medial lower leg; sensory loss to the anterior thigh and sometimes medial lower leg; hip flexion and adduction weakness, knee extension weakness; decreased patellar reflex.
-
L5 Nerve – back, radiating into buttock, lateral thigh, lateral calf and dorsum foot, great toe; sensory loss on the lateral calf, dorsum of the foot, webspace between first and second toe; weakness on hip abduction, knee flexion, foot dorsiflexion, toe extension and flexion, foot inversion and eversion; decreased semitendinosus/semimembranosus reflex.
-
S1 Nerve – back, radiating into buttock, lateral or posterior thigh, posterior calf, lateral or plantar foot; sensory loss on the posterior calf, lateral or plantar aspect of foot; weakness on hip extension, knee flexion, plantar flexion of the foot; Achilles tendon; Medial buttock, perineal, and perianal region; weakness may be minimal, with urinary and fecal incontinence as well as sexual dysfunction.
-
S2-S4 Nerves – sacral or buttock pain radiating into the posterior aspect of the leg or the perineum; sensory deficit on the medial buttock, perineal, and perianal region; absent bulbocavernosus, anal wink reflex.
-
Motor exam
-
Ankle dorsiflexion (L4 or L5)
-
Test by having the patient walk on heels
-
EHL weakness (L5)
-
Manual testing
-
Hip abduction weakness (L5)
-
Have the patient lie on the side on the exam table and abduct leg against resistance
-
Ankle plantarflexion (S1)
-
Have the patient do 10 single leg toes stand
Manual Test For collapsed disc
Straight Leg Raise ( SLR)
The Straight Leg Raise (SLR) test is a neurodynamic test. SLR is a neural tension test that can be used to rule in or out neural tissue involvement as a result of a space-occupying lesion, often a lumbar disc herniation collapsed disc. It is one of the most common neurological tests of the lower limb.

- A tension sign for L5 and S1 nerve root
- Can be done sitting or supine
- Reproduces pain and paresthesia in the leg at 30-70 degrees hip flexion
- Sensitivity/specificity most important and predictive physical finding for identifying who is a good candidate for surgery.
Contralateral SLR
- Crossed straight leg raise is less sensitive but more specific. Radicular pain in the affected leg when the contralateral asymptomatic leg is similarly raised constitutes a positive crossed straight-leg raise (X-SLR) test.
League Sign
- SLR aggravated by forced ankle dorsiflexion. Lasegue sign or straight leg raising test (SLRT) is a neurodynamic exam to assess nerve root irritation, posterior displacement, collapsed disc in the lumbosacral area.[rx] It is an integral element to the neurological exam for patients presenting with low back pain with or without radicular pain. The other less commonly used name is the Lazarevic sign.
Kernig Test
- Pain reproduced with neck flexion, hip flexion, and leg extension. Kernig’s sign is a test used in physical examination to look for evidence of irritation of the meninges, collapsed disc. The test involves flexing the thighs at the hip, and the knees, at 90-degree angles, and assessing whether the subsequent extension of the knee is painful (leading to resistance), in which case it is deemed positive.
Naffziger Test
A maneuver used to identify compression of nerve roots, collapsed disc in the cervical spine, based on exacerbation of pain and paraesthesias of the hand and fingers, when the examiner exerts pressure on the scalenus anterior muscles in patients with scalenus anterior syndrome. (for nerve root compression) increase or aggravation of pain or sensory disturbance over the distribution of the involved nerve root upon manual compression of the jugular veins bilaterally confirms the presence of an extruded intervertebral disk or other mass.
- Pain reproduced by coughing, which is instigated by lying patient supine and applying pressure on the neck veins Milgram test
- Pain reproduced with straight leg elevation for 30 seconds in the supine position
- Gait analysis
- Trendelenburg gait due to gluteus medius weakness which is innervated by L5.
Quadrant Test
- Position of patient – Standing
- Position of examiner – Standing behind the patient
- Procedure – Keep one hand over the patient’s contralateral shoulder and apply axial pressure. Ask the patient to hyperextend, rotate and laterally flex to the contralateral side.
- Interpretation – Provocative pain is taken as a sign of lumbar instability.
- Use – Used if pain cannot be produced by forwarding flexion, lateral flexion etc.
Adams Forward Bending Test
- Position of patient – Standing with feet together, knee extended.
- Position of examiner – Standing behind the patient first then in front of the patient.
- Procedure – Rule out limb length discrepancy. Ask the patient to bend forwards at the waist till the back is in the horizontal plane. Palms should be held together.
- Interpretation – If there is a rib or loin hump present, then there is structural scoliosis with rotation.
- Use – To differentiate between structural and non-structural scoliosis.
- Validity of test – For a patient with 40 structural scolioses, the test has a sensitivity of 0.83 and a specificity of 0.99.
Additional manual test for nerve root compression
- Crossed SLRT – AKA well-leg raising test or Fajersztajn sign. When the contralateral leg is lifted, the patient experiences pain on the affected side. [rx][rx]This test is more specific than ipsilateral SLRT. It becomes positive, usually in severe compression and centrally located prolapse. Fajersztajn believed that this sign is due to disc prolapse, in the axilla of the root.[rx]
- Reverse SLRT – AKA femoral stretch test. While the patient is in a prone position, the leg is lifted off the table with both hip and knee joints extended. Some authors may allow knee flexion. This maneuver may reproduce radicular pain in the case of upper lumbar radiculopathy, far lateral lumbar disc, or femoral neuropathy. The pain will present in the femoral nerve distribution on the side of the lesion.[rx]
- Ely’s test or Duncan-Ely test – is used to assess rectus femoris spasticity or tightness. The patient lies prone in a relaxed state. The therapist is standing next to the patient, at the side of the leg that will be tested. One hand should be on the lower back, the other holding the leg at the heel. Passively flex the knee in a rapid fashion. The heel should touch the buttocks. Test both sides for comparison. The test is positive when the heel cannot touch the buttocks, the hip of the tested side rises up from the table, the patient feels pain or tingling in the back or legs.
- Braggart test – AKA Sciatic stretch test or Flip test. While raising the leg, the foot is held in a dorsiflexed position so that the sciatic nerve is stretched more, thereby increasing the intensity of pain or making it possible to elicit the sign early.[rx][rx]
- Reverse flip test – While raising the leg, the foot is held in a plantar-flexed position; this will lessen the pain. But if the patient is complaining of an increase in pain, it can suggest malingering.[rx]
- Bowstring sign – Also known as the popliteal compression test or posterior tibial nerve stretch sign. The patient can be examined in sitting or in a supine position. The examiner flexes the knee and applies pressure on the popliteal fossa, evoking sciatica. Some examiners do it after SLRT by flexing the knee to relieve the buttock pain. The pain would be reproduced by a quick snap on the posterior tibial nerve in the popliteal fossa.[rx]
- The five repetitive sit-to-stand tests (5R-STS) – wherein a patient with the ability to perform the test in around 10 seconds does not rate as having a significant functional impairment.[rx]
Less Frequently Used Nerve Root Irritation Tests For collapsed disc
For the sake of completion, other tests and signs of nerve root tension or irritation are discussed succinctly below
-
Sitting SLRT (Bechterew test) – the patient is made to sit at the edge of a table with both hip and knee flexed, then made to extend the knee joint or elevate the extended knee, which reproduces the radicular pain and . They may be able to extend each leg alone, but extending both together causes radicular pain.[rx]
-
Distracted SLRT – the sitting SLRT is performed without the patient’s awareness. The patient is distracted as if the surgeon is examining the foot or pulsation, and slowly, the examiner extends the knee. If the patient is experiencing true radiculopathy, the same pain will be reproduced. Otherwise, we can assume that the patient may be malingering.
- Lasègue’s sign, Lasègue test or Lazarević’s sign – is a test done during a physical examination to determine whether a patient with low back pain has an underlying nerve root sensitivity, often located at L5 (fifth lumbar spinal nerve). With the patient lying down on their back on an examination table or exam floor, the examiner lifts the patient’s leg while the knee is straight. A variation is to lift the leg while the patient is sitting.[rx] However, this reduces the sensitivity of the test.[rx] In order to make this test more specific, the ankle can be dorsiflexed and the cervical spine flexed. This increases the stretching of the nerve root and dura.
- Neri’s sign – while bending forward, the patient flexes the knee to avoid stretching the nerve.[rx]
-
The buckling sign[rx] – the patient may flex the knee during SLRT to avoid sciatic nerve tension.
-
Sicard sign – passive dorsiflexion of ipsilateral great toe just at the angle of SLRT will produce more pain.
-
Kraus-Weber test – the patient may be able to do a sit-up with the knees flexed but not extended.
-
Minor sign – the patient may rise from a seated position by supporting himself/herself on the unaffected side, bending forward, and placing one hand on the affected side of the back.
-
Bonnet phenomenon – the pain may be more severe or elicited sooner if the test is carried out with the thigh and leg in a position of adduction and internal rotation.[rx]
Provocative Tests In A Spinal Examination And collapsed disc
- Shoulder Abduction (Relief) sign – Active abduction of symptomatic arm achieved by patient placing their ipsilateral hand on their head. A positive test results in relief (or reduction) of cervical radicular symptoms.
- Neck Distraction test – Active distractive force is applied by the examiner while grasping the patient’s head under the occiput and chin. A positive test results in relief (or reduction) of cervical radicular symptoms.
- L’hermitte’s sign – Examiner passively flexes patient’s cervical spine. A positive test result is an electric shock-like sensation down the spine or extremities.
- Hoffman’s sign – Passive snapping flexion of distal phalanx of patient’s middle finger. A positive test results in flexion-adduction of the ipsilateral thumb and index finger.
- Adson’s test – Patient is instructed to inspire with chin elevated, and head rotated to the affected side. A positive test results in obliteration of radial pulse.
- The Spurling test – is designed to reproduce symptoms by compression of the affected nerve root. The cervical extension is used to induce/reproduce posterior bulging of the intervertebral disk. Rotation of the head causes narrowing of the neuroforamina in the cervical spine. Finally, axial compression is applied to amplify these effects with the aim of exaggerating the preexisting nerve root compression.
- The prone instability test – The patient starts by standing on one end of the examination couch. While continuing to stand on the foot end of the couch, the patient lowers his / her torso onto the couch. The patient can hold onto the couch’s sides for support. The examiner then palpates the lower lumbar spine to elicit tenderness. The patient then holds onto the couch and lifts his / her feet off the ground tensing the paraspinal muscles. Less pain and tenderness on repeat palpation of the lower lumbar spine, while the feet are off the floor, is considered positive. [rx]
- Prone Plank/Bridge – The patient is prone and elevates his / her entire body off the couch/mat on forearms and tips of toes. The body should be parallel to the couch/mat. With adequate muscle strength, men should maintain this position for 124 +/- 72s and Women for 83 +/- 63s.[rx]
- Supine Bridge – The patient is supine and flexes the hip and knee to keep the feet flat on the couch/mat. The arms are flexed to position the hands beside the ears. The lower part of the torso and pelvis is lifted off the couch/mat, to maintain the trunk and the thigh in a straight line. With adequate muscle strength, men should maintain this position for 188 +/- 45s and Women for 152 +/- 30s. [rx]
Clinical Tests For Instability For collapsed disc
- Aberrant movement on flexion-extension – The standard examination involves documenting the range of movement. The quantitative range of movement may not be as significant as the qualitative range of movement. The important feature of spinal instability is the aberrant motion that occurs when flexing and extending the spine. A catch, a painful arc, supporting the arms on the thighs, or a reversal of the lumbopelvic rhythm when standing from the flexed posture indicates instability.[rx]
- Passive lumbar extension test – The subject lies on the examination couch. The examiner passively lifts the lower limbs to a height of 30 cm from the coach while maintaining the knee in extension and applying gentle traction on the legs. A positive test is recorded if the patient complains of “pain in the lower back region” or complains of “heaviness in the lower back” or complains that, “the lower back is coming off.” These experiences should return to normal when the leg returned to the couch. The passive lumbar extension test has the highest combined sensitivity and specificity and may be comparable to radiological findings to identify lumbosacral structural instability.[rx]
- The prone instability test – The patient stands at the foot end of the examination couch. The patient then lowers his/her upper body to rest on the examination couch. The iliac crest should rest on the edge of the examination couch. The patient holds the sides of the examination couch for increased stability. In the first part of the test, the feet of the patient is resting on the ground. The examiner with the heel of his/her hand creates a small posterior to anterior trust at each segment of the lumbar spine. Pain, if experienced by the patient, is recorded. In the second part of the test, the patient is asked to lift the feet of the floor and steady himself /herself by holding onto the sides of the examination couch. The examiner again repeats the posterior to anterior trust with the heel of his/her hand at each lumbar segment. The test is positive if the pain created in the initial part of the test subsides when the extensor muscles of the spine are tensed by lifting the feet of the floor.[rx]
Clinical Tests For Endurance In collapsed disc
- Sorensen test – The legs of the patient are strapped onto a low platform, which is only 25 cms above the floor. The upper end of the iliac crest is aligned to the edge of the table. The upper torso rests on the floor. At the commencement of the test, the patient extends the spine and lifts the upper torso off the floor with the arms crossed across the chest, and is asked to maintain the horizontal position. The record of the time, the patient can maintain this position is documented. Normative values: Men 146 +/- 51. Women 189 +/- 60.[rx]
- Prone isometric chest raise – The patient lies prone on the examination couch with a pad underneath the abdomen and the arms along the sides. The patient is instructed to lift the upper trunk about 30 degrees from the table while keeping the neck flexed, and the intention is to hold the sternum of the surface of the couch. The clinician records the maximum time that the patient can hold this position. [rx]Normative values: Men 40 +/- 9. Women 52 +/- 18.[rx]
- Prone double straight leg raise – The patient lies prone on the examination couch with the hips extended and the hands underneath the forehead. The arms are perpendicular to the body. The patient is then requested to lift both the legs off the couch until the knee is cleared off the couch. The patient should maintain normal breathing during the entire test procedure. The examiner can monitor the knee clearance by sliding a hand under the knee. The clinician records the maximum time that the patient can hold this position. Normative values: Men 38 +/- 6. Women 35 +/- 5. The prone double straight leg raise has shown to have great sensitivity and specificity. [rx]
- Supine static chest raise – The patient lies supine on the couch with the legs extended. The hands are placed on the temples with the elbows pointing to the ceiling. The patient is then instructed to lift the head, the arms and the upper trunk of the couch. The patient should maintain normal breathing during the entire test procedure. The clinician records the maximum time that the patient can hold this position. Normative values: Men 43 +/- 9. Women 32 +/- 5. [rx]
- Supine double straight leg raise – The patient lies supine with the legs extended, and the arms crossed in front of the chest. The pelvis is tilted forward to increase the lumbar lordosis. The patient is then requested to lift both the legs of the floor for 30 degrees while maintaining normal breathing during the entire test procedure. To monitor the pelvic tilt, the examiner can place one hand under the lumbar spine. The clinician records the maximum time that the patient can hold this position. Normative values: Men 28 +/- 4. Women 28 +/- 4. [rx]
- Flexor endurance test – The patient is supine on the couch with the upper part of the body propped up on a support. The support is at an angle of 60 degrees. The legs are flexed so that the knee is at a 90-degree angle with the foot flat on the couch. The toes and feet are strapped to the couch to provide a counterbalance. In a modified procedure, the examiner sits on the edge of the couch and over the toes of the patient to provide a counterbalance. The arms are crossed across the chest towards the opposite shoulder. The support is moved back by 10 cms, and the patient is instructed to maintain the original position. The clinician records the maximum time that the patient can hold this position. Normal values: Men 144 +/- 76, Women 149 +/- 99 in normal subjects.[rx]
- Prone Plank/Bridge – The patient lies prone on a mat. Initially, the patient lifts his / her upper torso off the mat and steadies on the elbows and forearms. The elbow is directly below the shoulder, and the forearms are straight with hands in front of the elbow. The patient then lifts the pelvis off the mat. The body is now supported on the elbow/forearm and the tips of the toes. The patient maintains a rigid horizontal position parallel to the floor. The clinician records the maximum time that the patient can hold this position. Normative values: Men 124 +/- 72s, Women 83 +/- 63s.[rx]
- Supine Bridge – The patient lies supine with the legs flexed so that the knee is at a 90-degree angle, and the foot is flat on the couch but not touching each other. The elbows are bent, and the hands are placed on the ears. The patient then lifts the pelvis so that the shoulders, hips, and knees are in a straight line. A rigid position is maintained, and the clinician records the maximum time that the patient can hold this position. Normative values: Men 188 +/- 45s, Women 152 +/- 30s.[rx]
- Side Plank/Bridge – The patient lies on the side on a mat. The upper part of the body is lifted off the mat and supported on the elbow of the arm below. The opposite (upper) arm crosses across the chest onto the lower shoulder. The top foot is positioned in front of the lower foot. The patient is then instructed to lift the pelvis off the floor and to maintain the trunk and the legs in a straight line. A rigid position is maintained, and the clinician records the maximum time that the patient can hold this position. Normative values: Men 95 +/- 35s, Women 74 +/- 33s.[rx]
Waddell Signs For Collapsed disc Include
-
Superficial tenderness – The patient’s skin over a wide area of the lumbar skin is tender to light touch or pinch.
-
Non-anatomical tenderness – The patient experiences deep tenderness over a wide area that is not localized to one structure and crosses over non-anatomical boundaries.
-
Axial loading – Downward pressure on the top of the patient’s head elicits lumbar pain.
-
Acetabular rotation – Lumbar pain is elicited while the provider passively and simultaneously externally rotates the patient’s shoulder and pelvis together in the same plane as the patient stands. It is considered a positive test if pain occurs within the first 30 degrees of rotation.
-
Distracted straight leg raises discrepancy – The patient complains of pain during a straight leg raise during formal testing, such as when supine, but does not on distraction when the examiner extends the knee with the patient in a seated position.
-
Regional sensory disturbance –The patient experiences decreased sensation fitting a stocking-like distribution rather than a dermatomal pattern.
-
Regional weakness – Weakness, cogwheeling, or the giving way of many muscle groups that are not explained on a neuroanatomical basis.
Observation of posture and function for Diagnosis of a collapsed disc
- In standing her shoulders lumbar paraspinal muscles – It is shunted to the left side, her back was extended and pelvis anteriorly tilted, and there was visible hyper-tonicity of the lumbar paraspinal muscles weakness in PLID, collapsed disc.
- This shunted antalgic posture – is commonly referred to as a lumber list. Observation of a lumber list, unfortunately, is a test lacking in reliability (Clare, Adams, & Maher, 2003). Maitland (2005), however, teaches us that if a person presents with an observable postural deformity in PLID, herniated disc, they are going to be more challenging to get better. In Sally’s case, she had a contralateral list (shoulders listed to the opposite side of back/leg pain), which is thought to respond more favorably to treatment than an ipsilateral list.
- Kyphosis-lordosis posture– Head held forwards, neck hyperextended, thoracic spine in long kyphosis, lumbar spine lordotic, pelvis tilted anteriorly, hips flexed, and knees hyperextended.
- Swayback posture– Head held forwards, neck hyperextended, thoracic spine in long kyphosis, lumbar spine flattened or slightly flexed, pelvis tilted posteriorly, hips hyperextended, knees hyperextended and ankle in neutral.
- Military type posture– Head neutral, neck straight, thoracic spine neutral or flattened, lumbar spine hyperextended, pelvis tilted anteriorly, knees hyperextended and ankles slightly plantarflexed.
- Flatback posture– Head held forwards, neck slightly extended, upper thoracic spine flexed, lower thoracic spine and lumbar spine flattened, pelvis tilted posteriorly, hips extended, knees hyperextended with plantarflexed ankles or knee flexed with the ankle in dorsiflexion.
- Femoral stretch test – While lying face down, your doctor will flex each knee to determine if you feel pain in your thigh. If you do, this indicates nerve compression in your lumbar spine.
- Schober test – This test examines the range of motion in your lumbar spine. During this test, you will bend over, as if you are trying to touch your toes.
- Trendelenburg test – This test can identify weakness in the muscles that support the hip. In this test, you’ll stand straight on one leg for 30 seconds. Your doctor will observe if your pelvis stays level.
- In my experience antalgic postures – are very important to detect because they indicate a protective position; a mechanism which the body is adopting (often subconsciously) in the acute phase of injury to protect the injury, and if the antalgic posture is not carefully examined and carefully corrected, it can make the patient a lot worse.
- Movement tests – Tests that assess the spine’s range of motion may include bending the neck or torso forward, backward, or to the side. Additionally, if raising one leg in front of the body worsens leg pain, it can indicate a lumbar herniated disc (straight leg raise test).
- Muscle strength – A neurological exam may be conducted to assess muscle strength and determine if a nerve root is compressed by a herniated disc. A muscle strength test may include holding the arms or legs out to the side or front of the body to check for tremors, muscle atrophy, or other abnormal movements.
- Reflex test – Nerve root irritation can dampen reflexes in the arms or legs. A reflex test involves tapping specific areas with a reflex hammer. If there is little or no reaction, it may indicate a compressed nerve root in the spine.
Active Range Of Movement
- Lumbar flexion P2 (right-sided low back pain) R`(upper thigh).
- Extension P2 (right buttock and leg pain) R` (vertical).
- Other movements were not assessed on day 1 due to severity and irritability.
Neurological Examination
- Weak single leg calf raises (SLCR) and was only able to perform three assisted raises to 50% range. Gr 5 strength of right leg SLCR x5 repetitions.
- No other myotomal weakness was detected.
- The S1 reflex on the right side was absent, with other lower limb reflexes being preserved.
- No sensory changes were noted.
Neurodynamic Examination
- The straight leg raise test (SLR) was positive in reproducing Sally’s posterior thigh pain and limited at 20 degrees on the right side.
- Her left SLR was limited by hamstring tightness at 50 degrees.
- The research suggests the SLR reliable re-assessment asterisks for patient progress. It has been shown to be 91% sensitive and 26% specific in detecting lumbar disc pathology. D Neville et al. (2020) found that more than an 11-degree discrepancy in hip flexion range between sides was a clinically significant result. Compared to MRI, the SLR test has poor diagnostic accuracy and therefore is often used in conjunction with such imaging.
Location of Pain and Motor Deficits in Association with Nerve Root Involvement at Each Lumbar Disc Level
| DISC LEVEL | LOCATION OF PAIN | MOTOR DEFICIT |
|---|---|---|
|
T12-L1 |
Pain in the inguinal region and medial thigh |
None |
|
L1-2 |
Pain in the anterior and medial aspect of the upper thigh |
Slight weakness in quadriceps; slightly diminished suprapatellar reflex |
|
L2-3 |
Pain in the anterolateral thigh |
Weakened quadriceps; diminished patellar or suprapatellar reflex |
|
L3-4 |
Pain in the posterolateral thigh and anterior tibial area |
Weakened quadriceps; diminished patellar reflex |
|
L4-5 |
Pain in the dorsum of the foot |
Extensor weakness of big toe and foot |
|
L5-S1 |
Pain in the lateral aspect of the foot |
Diminished or absent Achilles reflex |
Lab Test For Diagnosis of
A doctor can diagnose cauda’s low back pain or Collapsed Disc. Here’s what you may need to confirm a diagnosis
- Laboratory testing – may include white blood cell (WBC) count, erythrocyte sedimentation rate (ESR), and C-reactive protein (CRP).
- Elevated ESR – could indicate infection, malignancy, chronic disease, inflammation, trauma, or tissue ischemia.
- Elevated CRP – levels are associated with infection.
- RBS – To diagnosis, diabetes and it related health problem, burning sensation, etc
- Rheumatoid factor and anti-CCP – cyclic citrullinated peptide antibodies test should be increased if there is clinical abnormality for PLID, collapsed disc, or right and left side back pain are found.
- A serum uric acid level – It is often considered by clinicians and doctors when PLID, collapsed disc is suspected, but it is not a reliable and dangerous condition of your kidney as it may be spuriously elevated or high in acute inflammatory conditions or acutely during an attack or not.
- Serologic studies – There are no blood tests used to specifically support the diagnosis of nerve compression, collapsed disc, demyelination but the use of these tests may be necessary for medical conditions that can either increase nerve compression or can decrease their symptoms. Some of the most frequently find conditions include diabetes and hypothyroidism. The assessment of a patient’s fasting blood glucose, hemoglobin A1c, or thyroid function tests may be helpful in the general management of the patient. Other conditions that could mimic nerve compression include deficiency of vitamin B12 or folate, vasculitides, and fibromyalgia.
- Synovial fluid analysis – A joint arthrocentesis or the system of aspiration of synovial fluid with blood and synovial fluid analysis that are mandatory if an infection is suspected or dangerous. The fluid analysis or any kind of abnormalities is also helpful in diagnosing crystal formation with osteophyte and steroid-induced arthritis. The degree of the high elevation of synovial fluid are founded by WBC count can be useful in differentiating inflammatory abnormality or from non-inflammatory causes of right and left side neck pain.
Imaging Test For collapsed disc
- X-rays – can show the alignment of the bones and whether the patient has arthritis or broken bones. They are not ideal for detecting problems with muscles, the spinal cord, nerves, or disks, collapsed discs.
- Computed Tomography (CT) scan – is a noninvasive test that uses an X-ray beam and a computer to make 2-dimensional images of your spine. It may or may not be performed with a dye (contrast agent) injected into your bloodstream. This test is especially useful for confirming which bulging disc, is damage and is good for revealing herniated disks or problems with tissue, tendons, nerves, ligaments, blood vessels, muscles, and bones.
- Bone scan – a bone scan may be used for detecting bone tumors or compression fractures caused by brittle bones (osteoporosis). The patient receives an injection of a tracer (a radioactive substance) into a vein. The tracer collects in the bones and helps the doctor detect bone problems with the aid of a special camera.
- Magnetic Resonance Imaging (MRI) scan – is a noninvasive test that uses a magnetic field and radiofrequency waves to give a detailed view of the soft tissues of your spine with a bulging disc, collapsed disc. Unlike an X-ray, nerves and discs are clearly visible. It may or may not be performed with a dye (contrast agent) injected into your bloodstream. An MRI can detect which disc is damaged and if there is any nerve compression. It can also detect bony overgrowth, spinal cord tumors, or abscesses.
- Nuclear Magnetic resonance imaging (MRI) scan – which uses magnetic fields and computers to produce three-dimensional images of your spine.
- A myelogram – is a specialized X-ray where dye is injected into the spinal canal through a spinal tap. An X-ray fluoroscope then records the images formed by the dye. The dye used in a myelogram shows up white on the X-ray, allowing the doctor to view the spinal cord and canal, PLID, a bulging disc in detail. Myelograms can show a nerve being pinched and a bulging disc by a herniated disc, bony overgrowth, spinal cord tumors, and abscesses.
- Electromyography (EMG) & Nerve Conduction Studies (NCS) – EMG tests measure the electrical activity of your muscles. Small needles are placed in your muscles, and the results are recorded on a special machine. NCS is similar, but it measures how well your nerves pass an electrical signal from one end of the nerve to another. These tests can detect nerve damage and muscle weakness and a bulging disc, collapsed disc, and PLID. [rx][rx]
- Discogram – A discogram may be recommended to confirm which bulging disc and PLID is painful if surgical treatment is considered. In this test, the radiographic dye is injected into the disc to recreate disc pain from the dye’s added pressure. It is useful for the evaluation of patients who are experiencing cervical discogenic pain or have multiple herniations in which surgery is a strong possibility. However, the diagnostic procedure remains controversial as it may accelerate the degeneration of normal discs.[rx]
- CT myelogram – CT is most useful when combined with the injection of intrathecal contrast (myelography) to better evaluate the location and amount of neural compression. It is more invasive than an MRI but can be a consideration in patients who have a contraindication to MRI (e.g., pacemaker) or have an artifact from the hardware.
- Cerebrospinal fluid analysis – is a useful test if there is a suspected neoplasm or infectious cause or radiculopathy symptoms. The recommendation for a lumbar puncture is in the case of a patient with negative or nondiagnostic neuroimaging, without known primary cancer, who has progressive neurological symptoms and has failed to improve promptly.[rx]
- Bone scintigraphy – with single-photon emission computed tomography (SPECT) is more sensitive in detecting facet joint lesions and allows more accurate anatomical localization. A recent study suggested that SPECT could help to identify patients with low back pain, PLID who would benefit from facet joint injections [rx].
- Foraminal nerve root entrapment test – is best visualized on T1-weighted MRI where the high contrast between fat tissue and the nerve root sheath is of great help. Usually, a combination of hypertrophic degenerative facets with osteophytes spurs posteriorly, and vertebral osteophytes and PLID/collapsed disc or disc herniation anteriorly diminish the anteroposterior diameter of the foramen. Foraminal height is lessened by degenerative disc disease and subsequent disc height loss. Whenever the normal rounded (oval) appearance of the nerve root sheath is lost in combination with loss of the surrounding fat tissue, nerve root compression should be considered.
- Urodynamic studies – may be required to monitor the recovery of bladder function following decompression surgery.
- Electrodiagnostic studies – Electromyography and nerve conduction test studies help to localize the nerve problem involved as well as where along the course of the nerve it is affected. Additionally, testing can serve as a baseline for comparison with the future during the course of treatment. It is important to note that normal electrodiagnostic studies do not identify disease, and clinical correlation should include the patient’s history and physical examination findings.[rx]
In most cases of low back pain, medical consensus advises not seeking an exact diagnosis but instead beginning to treat the pain. This assumes that there is no reason to expect that the person has an underlying problem. In most cases, the pain goes away naturally after a few weeks. Typically, people who do seek diagnosis through imaging are not likely to have a better outcome than those who wait for the condition to resolve.
Treatment Of Posterior Displacement of C5 Vertebra
Patient Education
-
Use of hot or cold packs for comfort and to decreased inflammation
-
Avoidance of inciting activities or prolonged sitting/standing
-
Practicing good, erect posture
-
Engaging in exercises to increase core strength
-
Gentle stretching of the lumbar spine and hamstrings
-
Regular light exercises such as walking, swimming, or aromatherapy
-
Use of proper lifting techniques
Non-Pharmacological Treatment
Conservative Treatments – Acute cervical or lumbar radiculopathies and collapsed disc secondary to a herniated disc are typically managed with non-surgical treatments as the majority of patients (75 to 90%) will improve. Modalities that can be used include[rx][rx][rx]:
- Rest the area by avoiding any activity that causes worsening symptoms in the arms or legs.
- Stay active around the house, and go on short walks several times per day. The movement will decrease pain and stiffness and help you feel better.
- Apply ice packs to the affected area for 15 to 20 minutes every 2 hours.
- Sit in firm chairs. Soft couches and easy chairs may make your problems worse.
-
Deep tissue massage may be helpful in collapsed disc
-
Acupuncture – In acupuncture, the therapist inserts fine needles into certain points on the body with the aim of relieving pain.
-
Reiki – Reiki is a Japanese treatment that aims to relieve pain by using specific hand placements.
-
Moxibustion – This method is used to heat specific parts of the body (called “therapy points”) by using glowing sticks made of mugwort (“Moxa”) or heated needles that are put close to the therapy points.
-
Massages – Various massage techniques are used to relax muscles and ease tension. Massage is the practice of applying structured or unstructured pressure, tension, movement, or vibration – manually or with mechanical assistance – to the soft tissues of the body, including the skin, muscles, connective tissue, tendons, ligaments, joints, etc. lymphatic vessels, organs of the gastrointestinal and reproductive system, to increase any aspect of the well-being of the masses (that is: the one being massaged). This can be done with or without massage oil.
- Heating and cooling – This includes the use of hot packs and plasters, a hot bath, going to the sauna, or using an infrared lamp. Heat can also help relax tense muscles. Cold packs, like cold wraps or gel packs, are also used to help with irritated nerves. Heat and Ice therapy is one of the conservative treatments patients do to relieve themselves of the symptoms of a collapsed disc condition.
- Heat Therapy – It is also known as thermotherapy. It is especially helpful in treating localized pain caused by the herniated disc and muscle spasms. The heat helps blood flow and oxygen to relax the affected areas. It alleviates certain if not all discomforts caused by the disc herniation. One can use heat packs and hot towels.
- Ice Therapy – It is also known as cryotherapy. It is especially helpful in reducing the inflammation caused by the affected nerve from the herniated disc. One can use ice or cold gel packs. Basically, it is a combination of both heat and ice therapies. It is reported that the combination of both is actually more effective in administering relief to the pain caused by the herniated discs. However, it is dependent on the individual as some can render more pain too since inflammation cannot be suited by heat and neither can muscle spasms.
-
Ultrasound therapy – Here the lower back is treated with sound waves. The small vibrations that are produced generate heat to relax body tissue.
-
Cervical Manipulation – There is limited evidence suggesting that cervical manipulation may provide short-term benefits for neck pain and cervicogenic headaches. Complications from manipulation are rare and can include worsening radiculopathy, myelopathy, spinal cord injury, and vertebral artery injury. These complications occur ranging from 5 to 10 per 10 million manipulations.
-
Lumbar Corset or Collar for Immobilization – In patients with acute neck pain, a short course (approximately one week) of collar immobilization may be beneficial during the acute inflammatory period.
- Traction – This May be beneficial in reducing the radicular symptoms associated with disc herniations. Theoretically, traction would widen the neuroforamen and relieve the stress placed on the affected nerve, which, in turn, would result in the improvement of symptoms. This therapy involves placing approximately 8 to 12 lbs of traction at an angle of approximately 24 degrees of neck flexion over a period of 15 to 20 minutes.
Physical Therapy
- Exercising in water – can be a great way to stay physically active when other forms of exercise are painful. Exercises that involve lots of twisting and bending may or may not benefit you. Your physical therapist will design an individualized exercise program to meet your specific needs.
- Weight-training exercises – though very important, need to be done with proper form to avoid stress to the back and neck.
- Reduce pain and other symptoms – Your physical therapist will help you understand how to avoid or modify the activities that caused the injury, so healing can begin. Your physical therapist may use different types of treatments and technologies to control and reduce your pain and symptoms.
- Improve posture –If your physical therapist finds that poor posture has contributed to your herniated disc/slipped disc, the therapist will teach you how to improve your posture so that pressure is reduced in the injured area, and healing can begin and progress as rapidly as possible.
- Improve motion – Your physical therapist will choose specific activities and treatments to help restore normal movement in any stiff joints. These might begin with “passive” motions that the physical therapist performs for you to move your spine, and progress to “active” exercises and stretches that you do yourself. You can perform these motions at home and in your workplace to help hasten healing and pain relief.
- Improve flexibility – Your physical therapist will determine if any of the involved muscles are tight, start helping you to stretch them, and teach you how to stretch them at home.
- Improve strength – If your physical therapist finds any weak or injured muscles, your physical therapist will choose, and teach you, the correct exercises to steadily restore your strength and agility. For neck and back disc herniations, “core strengthening” is commonly used to restore the strength and coordination of muscles around your back, hips, abdomen, and pelvis.
- Improve endurance – Restoring muscular endurance is important after an injury. Your physical therapist will develop a program of activities to help you regain the endurance you had before the injury, and improve it.
- Learn a home program – Your physical therapist will teach you strengthening, stretching, and pain-reduction exercises to perform at home. These exercises will be specific for your needs; if you do them as prescribed by your physical therapist, you can speed your recovery.
Eat Nutritiously During Your Recovery
- All bones and tissues in the body need certain nutrients in order to heal properly and in a timely manner. Eating a nutritious and balanced diet that includes lots of minerals and vitamins are proven to help heal broken bones of all types. Therefore focus on eating lots of fresh produce (fruits and veggies), whole grains, lean meats, and fish to give your body the building blocks needed to properly repair your. In addition, drink plenty of purified water, milk, and other dairy-based beverages to augment what you eat.
- Broken bones need ample minerals (calcium, phosphorus, magnesium, boron) and protein to become strong and healthy again.
- Excellent sources of minerals/protein include dairy products, tofu, beans, broccoli, nuts and seeds, sardines, and salmon.
- Important vitamins that are needed for bone healing include vitamin C (needed to make collagen), vitamin D (crucial for mineral absorption), and vitamin K (binds calcium to bones and triggers collagen formation).
- Conversely, don’t consume food or drink that is known to impair bone/tissue healing, such as alcoholic beverages, sodas, most fast food items, and foods made with lots of refined sugars and preservatives.
Medication
Pharmacotherapy – There is no evidence to demonstrate the efficacy of non-steroidal anti-inflammatories (NSAIDs) in the treatment of collapsed discs. However, they are commonly used and can be beneficial for some patients. The use of COX-1 versus COX-2 inhibitors does not alter the analgesic effect, but there may be decreased gastrointestinal toxicity with the use of COX-2 inhibitors.
- Non-steroidal anti-inflammatory drugs (NSAIDs) – These painkillers belong to the same group of drugs as acetylsalicylic acid (ASA, the drug in medicines like “Aspirin”). NSAIDs that may be an option for the treatment of sciatica include diclofenac, ibuprofen, and naproxen. Anti-inflammatory drugs are drugs that reduce inflammation. This includes substances produced by the body itself like cortisone. It also includes artificial substances like ASA – acetylsalicylic acid (or “aspirin”) or ibuprofen –, which relieve pain and reduce fever as well as reducing inflammation.
-
Acetaminophen (paracetamol) – Acetaminophen (paracetamol) is also a painkiller, but it is not an NSAID. It is well tolerated and can be used as an alternative to NSAIDs – especially for people who do not tolerate NSAID painkillers because of things like stomach problems or asthma. But higher doses of acetaminophen can cause liver and kidney damage. The package insert advises adults not to take more than 4 grams (4000 mg) per day. This is the amount in, for example, 8 tablets containing 500 milligrams each. It is not only important to take the right dose, but also to wait long enough between doses.
-
Opioids – Strong painkillers that may only be used under medical supervision. Opioids are available in many different strengths, and some are available in the form of a patch. Morphine, for example, is a very strong drug, while tramadol is a weaker opioid. These drugs may have a number of different side effects, some of which are serious. They range from nausea, vomiting and constipation to dizziness, breathing problems, and blood pressure fluctuation. Taking these drugs for a long time can lead to habitual use and physical dependence.
- Skeletal Muscle relaxant – If muscle spasms are prominent, the addition of a muscle relaxant may merit consideration for a short period. For example, cyclobenzaprine is an option at a dose of 5 mg taken orally three times daily. Antidepressants (amitriptyline) and anticonvulsants (gabapentin and pregabalin) have been used to treat neuropathic pain, and they can provide a moderate analgesic effect.
-
Steroids – Anti-inflammatory drugs that can be used to treat various diseases systemically. That means that they are taken as tablets or injected. The drug spreads throughout the entire body to soothe inflammation and relieve pain. Steroids may increase the risk of gastric ulcers, osteoporosis, infections, skin problems, glaucoma, and glucose metabolism disorders.
-
Muscle relaxants – Sedatives that also relax the muscles. Like other psychotropic medications, they can cause fatigue and drowsiness, and affect your ability to drive. Muscle relaxants can also affect liver functions and cause gastro-intestinal complications. Drugs from the benzodiazepine group, such as tetrazepam, can lead to dependency if they are taken for longer than two weeks.
- Nerve Relaxant and Neuropathic Agents – Drugs(pregabalin & gabapentin) or Vitamin B1 B6, B12 and mecobalamin that address neuropathic—or nerve-related pain remover. This includes burning, numbness, and tingling.
-
Anticonvulsants – These medications are typically used to treat epilepsy, but some are approved for treating nerve pain (neuralgia). Their side effects include drowsiness and fatigue. This can affect your ability to drive.
- Antidepressants – These drugs are usually used for treating depression. Some of them are also approved for the treatment of pain. Possible side effects include nausea, dry mouth, low blood pressure, irregular heartbeat, and fatigue.
- Topical Medications – These prescription-strength creams, gels, ointments, patches, and sprays help relieve pain and inflammation through the skin.
- Calcium & vitamin D3 – to improve bone health and healing fracture. As a general rule, men and women age 50 and older should consume 1,200 milligrams of calcium a day, and 600 international units of vitamin D a day.
- Glucosamine & Diacerein, Chondroitin sulfate – can be used to tightening the loose tension, cartilage, ligament, and cartilage, ligament regenerate cartilage or inhabit the further degeneration of cartilage, ligament
- Injections near the spine – Injection therapy uses mostly local anesthetics and/or anti-inflammatory medications like corticosteroids (for example cortisone). These drugs are injected into the area immediately surrounding the affected nerve root. There are different ways of doing this:
-
In lumbar spinal nerve analgesia (LSPA) – the medication is injected directly at the point where the nerve root exits the spinal canal. This has a numbing effect on the nerve root.
-
In lumbar epidural analgesia – the medication is injected into what is known as the epidural space (“epidural injection”). The epidural space surrounds the spinal cord and the spinal fluid in the spinal canal. This is also where the nerve roots are located. During this treatment, the spine is monitored using computer tomography or X-rays to make sure that the injection is placed at exactly the right spot.
-
Interventional Treatments – Spinal steroid injections are a common alternative to surgery. Perineural injections (translaminar and transforaminal epidurals, selective nerve root blocks) are an option with pathological confirmation by MRI. These procedures should take place under radiologic guidance.[15]
-
Surgical Treatments
- Total Disc Replacement (TDR) and Anterior Cervical Discectomy and Fusion (ACDF) – Surgical exposure of the desired vertebral level is achieved through an anterior cervical incision. Subcutaneous dissection is performed to allow for adequate mobilization to tissue incision. The discectomy is performed with pituitary rongeurs, a curette, and a burr drill to remove the affected disc. The posterior longitudinal ligament can be left in situ depending on the severity of the herniation.
- Laminectomy – Cervical laminectomy removes the lamina on one or both sides to increase the axial space available for the spinal cord. Clinically indicated for spinal stenosis or cervical disc disease involving more than three levels of disc degeneration with anterior spinal cord compression. Single-level cervical disc herniation is usually managed with the anterior approach. The complications of the posterior approach include instability resulting in kyphosis, recalcitrant myofascial pain, and occipital headaches.
- Laminoplasty – The kyphotic deformity is a well-known complication of laminectomy. To preserve the posterior wall of the spinal canal while decompressing the spinal canal a Z-plasty technique for the lamina was developed. The variant of the procedure uses a hinged door for the lamina. Laminoplasty is commonly indicated for multilevel spondylotic myelopathy. Nerve root injury is seen in about 11% of the surgeries. This complication is unique to laminoplasty, and the suggested etiology is traction on the nerve root with the posterior migration of the spinal cord.[rx]
- Anterior cervical discectomy and fusion – A procedure that reaches the cervical spine (neck) through a small incision in the front of the neck. The intervertebral disc is removed and replaced with a small plug of bone or another graft substitute, and in time, that will fuse the vertebrae.
- Cervical corpectomy – A procedure that removes a portion of the vertebra and adjacent intervertebral discs to allow for decompression of the cervical spinal cord and spinal nerves. A bone graft, and in some cases a metal plate and screws, are used to stabilize the spine.
- Dynamic Stabilisation – Following a discectomy, a stabilization implant is implanted with a ‘dynamic’ component. This can be with the use of Pedicle screws (such as Dynesys or a flexible rod) or an interspinous spacer with bands (such as a Wallis ligament). These devices offload pressure from the disc by rerouting pressure through the posterior part of the spinal column. Like a fusion, these implants allow maintaining mobility to the segment by allowing flexion and extension.
- Facetectomy – A procedure that removes a part of the facet to increase the space.
- Foraminotomy – A procedure that enlarges the vertebral foramen to increase the size of the nerve pathway. This surgery can be done alone or with a laminotomy.
- Intervertebral disc annuloplasty (IDET) – A procedure wherein the disc is heated to 90 °C for 15 minutes in an effort to seal the disc and perhaps deaden nerves irritated by the degeneration.
- Intervertebral disc arthroplasty – also called Artificial Disc Replacement (ADR), or Total Disc Replacement (TDR), is a type of arthroplasty. It is a surgical procedure in which degenerated intervertebral discs in the spinal column are replaced with artificial ones in the lumbar (lower) or cervical (upper) spine.
- Laminoplasty – A procedure that reaches the cervical spine from the back of the neck. The spinal canal is then reconstructed to make more room for the spinal cord.
- Laminotomy – A procedure that removes only a small portion of the lamina to relieve pressure on the nerve roots.
- Microdiscectomy – A minimally invasive surgical procedure in which a portion of a herniated nucleus pulposus is removed by way of a surgical instrument or laser while using an operating microscope or loupe for magnification.
- Percutaneous disc decompression – A procedure that reduces or eliminates a small portion of the bulging disc through a needle inserted into the disc, minimally invasive.
- Spinal decompression – A non-invasive procedure that temporarily (a few hours) enlarges the intervertebral foramen (IVF) by aiding in the rehydration of the spinal discs.
- Spinal laminectomy – A procedure for treating spinal stenosis by relieving pressure on the spinal cord. A part of the lamina is removed or trimmed to widen the spinal canal and create more space for the spinal nerves.
Rehabilitation Posterior Displacement Vertebra
Physical Therapy Management
Physical therapy often plays a major role in Collapsed Disc recovery. Involving below key points
- Ambulation and resumption of exercise
- Pain control
- Education re maintaining a healthy weight
Physical therapy programs are often recommended for the treatment of pain and restoration of functional and neurological deficits associated with symptomatic disc herniation.
Active exercise therapy is preferred to passive modalities.
There are a number of exercise programs for the treatment of symptomatic disc herniation eg
- aerobic activity (eg, walking, cycling)
- directional preference (McKenzie approach)
- flexibility exercises (eg, yoga and stretching)
- proprioception/coordination/balance (medicine ball and wobble/tilt board),
- strengthening exercises.
- motor control exercises MCEs
MCEs (stabilization/core stability exercises) are a common type of therapeutic exercise prescribed for patients with symptomatic disc herniation[rx].
- designed to re-educate the co-activation pattern of abdominals, paraspinal, gluteals, pelvic floor musculature and diaphragm
- The biological rationale for MCEs is primarily based on the idea that the stability and control of the spine are altered in patients with LBP.
- the program begins with the recognition of the natural position of the spine (mid-range between lumbar flexion and extension range of motion), considered to be the position of balance and power for improving performance in various sports
- Initial low-level sustained isometric contraction of trunk-stabilizing musculature and their progressive integration into functional tasks is the requirement of MCEs
- MCE is usually delivered in 1:1 supervised treatment sessions and sometimes includes palpation, ultrasound imaging, and/or the use of pressure biofeedback units to provide feedback on the activation of trunk musculature
- A core stability program decreases pain level, improves functional status, increases the health-related quality of life, and static endurance of trunk muscles in lumbar disc herniation patients[rx]. Individual high-quality trials found moderate evidence that stabilization exercises are more effective than no treatment[rx].
Different studies have shown that a combination of different techniques will form the optimal treatment for a Collapsed Disc. Exercise and ergonomic programs should be considered as very important components of this combined therapy[rx].
Physiotherapy Modalities and the evidence for their use in disc herniation
- Stretching – There is low-quality evidence found to suggest that adding hyperextension to an intensive exercise program might not be more effective than intensive exercise alone for functional status or pain outcomes. There were also no clinically relevant or statistically significant differences found in disability and pain between combined strength training and stretching, and strength training alone[rx].
- Muscle Strengthening – Strong muscles are a great support system for your spine and better handle pain. If core stability is totally regained and fully under control, strength and power can be trained. But only when this is necessary for the patient’s functioning/activities. This power needs to be avoided during the core stability exercises because of the combination of its two components: force and velocity. This combination forms a higher risk to gain back problems and back pain[rx].
- Traditional Chinese Medicine for Low Back Pain – has been demonstrated to be effective. Reviews have demonstrated that acupressure, acupuncture, and cupping can be efficacious in pain and disability for chronic low back pain included disc herniation[rx][rx].
- Spinal Manipulative Therapy and Mobilization – Spinal manipulative therapy and mobilization lead to short-term pain relief when suffering from acute low back pain. When looking at chronic low back pain, manipulation has an effect similar to NSAID[rx].
- Behavioural Graded Activity Programme – A global perceived recovery was better after a standard physiotherapy program than after a behavioral graded activity program in the short term, however, no differences were noted in the long term[rx].
- Transcutaneous Electrical Nerve Stimulation (TENS) – TENS therapy contributes to pain relief and improvement of function and mobility of the lumbosacral spine[rx].
- Manipulative Treatment – Manipulative treatment on lumbar disc herniation appears to be safe, effective, and it seems to be better than other therapies. However high-quality evidence is needed to be further investigated[rx].
- Traction – A recent study has shown that traction therapy has positive effects on pain, disability, and SLR on patients with intervertebral disc herniation[rx]. Also, one trial found some additional benefit from adding mechanical traction to medication and electrotherapy[rx].
- Aquatic Vertical Traction – In patients with low back pain and signs of nerve root compression this method had greater effects on spinal height, the relieving of pain, lowering the centralization response, and lowering the intensity of pain than the assuming of a supine flexing position on land[rx].
- Hot Therapies – may use heat to increase blood flow to the target area. Blood helps heal the area by delivering extra oxygen and nutrients. Blood also removes waste byproducts from muscle spasms.
Example of Protocol for Rehabilitation Following a Lumbar Microdiscectomy
The following program is an example of a protocol for rehabilitation following a lumbar microdiscectomy
- Duration of a rehabilitation program – 4 weeks
- Frequency – every day
- Duration of one session – approximately 60 minutes
- Treatment – dynamic lumbar stabilization exercises + home exercises
- Exercises – Prior to the DLS training session patients are provided with instruction or techniques to ensure and protect a neutral spine position. During the first 15 minutes of each session stretching of back extensors, hip flexors, hamstrings and Achilles tendon should be performed.
- DLS consists of – Quadratus exercises Abdominal strengthening Bridging with ball Straightening of external abdominal oblique muscle Lifting one leg in crawling position Lifting crossed arms and legs in crawling position Lunges)
- Home Exercises – should be added to the treatment. These should be performed every day. 5 repetitions during the first week up to 10-15 reps in the following weeks
Post Surgical Intervention – In the case of surgery, programs start regularly 4-6 weeks post-surgery
- Offer information about the rehabilitation program they will follow in the next few weeks.
- The patients are instructed and accompanied in daily activities such as: coming out of bed, going to the bathroom, and clothing
- Patients have to pay attention to the ergonomics of the back throughout back school[rx][rx][rx][rx].
Studies show various forms of post-operation treatment show
- Rehabilitation programs that start four to six weeks post-surgery with exercises versus no treatment found that exercise programs are more effective than no treatment in terms of short-term follow-up for pain
- High-intensity exercise programs are slightly more effective for pain and in terms of functional status in the short term compared with low-intensity exercise programs.
- Long-term follow-up results for both pain and functional status showed no significant differences between groups.
- No significant differences between supervised exercise programs and home exercise programs in terms of short-term pain relief[rx].
Complications
Complications from steroid injections are typically mild and range between 3% to 35% of cases. Other, more serious complications can include[rx]
-
Nerve injury
-
Infection
-
Epidural hematoma
-
Epidural abscess
-
Spinal cord infarction
-
Bleeding
-
Recurrence of disease or symptoms
-
Infection
-
Worsening neurological deficits
-
Failed operation
Complications from surgical intervention include[rx]
-
Infection
-
Recurrent laryngeal, superior laryngeal, and hypoglossal nerve injuries
-
Esophageal injury
-
Vertebral and carotid injuries
-
Dysphagia
-
Horner syndrome
-
Pseudoarthrosis
-
Adjacent segment degeneration
A team approach is an ideal way to limit the complications of such an injury
-
Evaluation of a patient with lumbar radicular pain by the primary care provider to rule out severe radiculopathy or alarm symptoms is the recommended first step.
-
Conservative management should commence when symptoms are mild or moderate; including moderate activity, stretches, and pharmacological management. A pharmacist should evaluate dosing and perform medication reconciliation to preclude any drug-drug interactions, and alert the healthcare team regarding any concerns.
-
The patient should follow up with primary care physicians one to two weeks following initial injury to monitor for progression of the nerve damage.
-
If symptoms worsen on follow-up or there is a concern for the development of a severe radiculopathy referral to neurosurgery or hospitalization for possible spinal decompression.
-
If radicular symptoms persist three weeks after injury, physical therapy referral can be a consideration.
-
When symptoms persist for greater than six-week duration, imaging such as MRI or CT can are options for better visualization of the nerve roots.
-
The patient should consult with a dietitian and eat a healthy diet and maintain a healthy weight.
-
The pharmacist should encourage the patient to quit smoking, as this may help with the healing process. Further, the pharmacist should educate the patient on pain management and available options.
-
Persistent pain at six weeks follows up may warrant a referral to interventional pain management or neurosurgery for an epidural steroid injection.
-
If mild to moderate symptoms continue at three months following the onset of symptoms, referral for possible surgical intervention merits consideration as well.
Prevention
To prevent experiencing a herniated disc, individuals should:
- Use proper body mechanics when lifting, pushing, pulling, or performing any action that puts extra stress on your spine.
- Maintain a healthy weight. This will reduce the stress on your spine.
- Stop smoking.
- Discuss your occupation with a physical therapist, who can provide an analysis of your job tasks and offer suggestions for reducing your risk of injury.
- Keep your muscles strong and flexible. Participate in a consistent program of physical activity to maintain a healthy fitness level.
- Many physical therapy clinics offer “back schools,” which teach people how to take care of their backs and necks and prevent injury. Ask your physical therapist about programs in your area. If you don’t have a physical therapist.
To prevent recurrence of a herniated disc, follow the above advice, and:
- Continue the new posture and movement habits that you learned from your physical therapist, to keep your back healthy.
- Continue to do the home exercise program your physical therapist taught you, to help maintain your improvements.
- Continue to be physically active and stay fit.