Renal parenchymal disorders refer to a group of kidney conditions that affect the functional tissue of the kidneys, known as the parenchyma. These disorders can impact the kidneys’ ability to filter blood, maintain fluid and electrolyte balance, and produce essential hormones. Understanding renal parenchymal disorders is crucial for early detection, effective management, and prevention of kidney-related complications.
Renal parenchymal disorders encompass various conditions that damage the kidney’s functional tissue. These disorders can lead to impaired kidney function, chronic kidney disease (CKD), and eventually kidney failure if not managed properly. Common renal parenchymal disorders include glomerulonephritis, polycystic kidney disease, and acute tubular necrosis.
Anatomy of the urinary system | |||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Kidneys |
| ||||||||||||
| Ureters |
| ||||||||||||
| Bladder |
| ||||||||||||
| Urethra |
| ||||||||||||
A
- Afferent arterioles
- Arcuate arteries of the kidney
- Arcuate vein
- Ascending limb of loop of Henle
- Augmented renal clearance
B
- Bowman’s capsule
- Brodel’s bloodless line
C
- Collecting duct system
- Cortical lobule
- Crossed renal ectopia
D
- Descending limb of loop of Henle
- Distal convoluted tubule
E
- Ectopic kidney
- Efferent arteriole
G
- Glomerular basement membrane
- Glomerulus (kidney)
I
- Interlobar arteries
- Interlobar veins
- Interlobular arteries
- Interlobular veins
- Intraglomerular mesangial cell
J
- Juxtaglomerular apparatus
- Juxtaglomerular cell
- Juxtamedullary nephron
L
- Loop of Henle
M
- Macula densa
- Medullary ray (anatomy)
N
- Nephron
P
- Papillary duct
- Peritubular capillaries
- Podocyte
- Precision cut kidney slices
- Proximal tubule
R
- Renal calyx
- Renal capsule
- Renal circulation
- Renal column
- Renal corpuscle
- Renal cortex
- Renal fascia
- Renal hilum
- Renal lobe
- Renal medulla
- Renal papilla
- Renal pelvis
- Renal pyramids
- Renal sinus
S
- Segmental arteries of kidney
- Stellate veins
T
- Thin segment of loop of Henle
V
- Vasa recta (kidney)
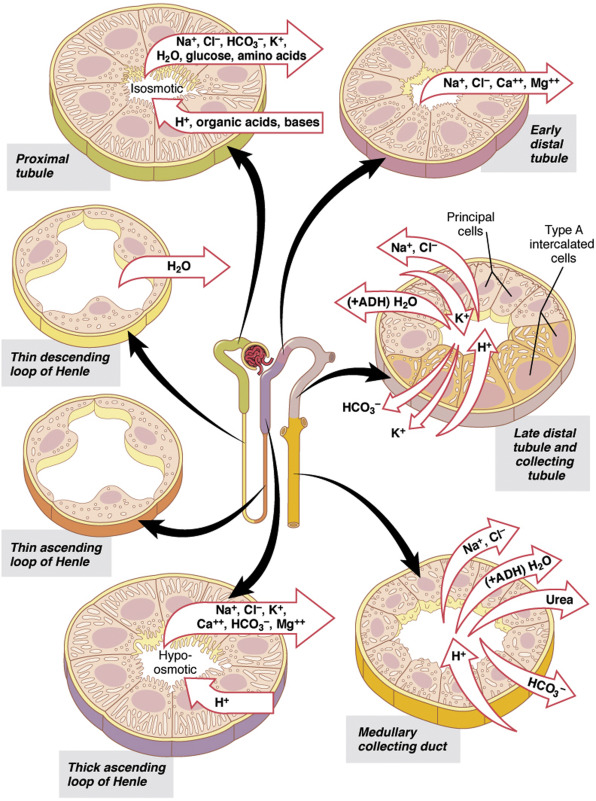
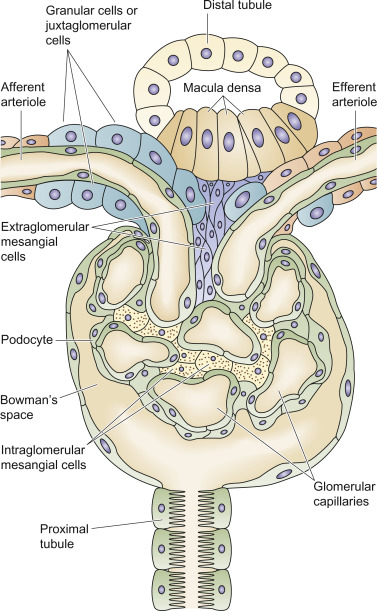
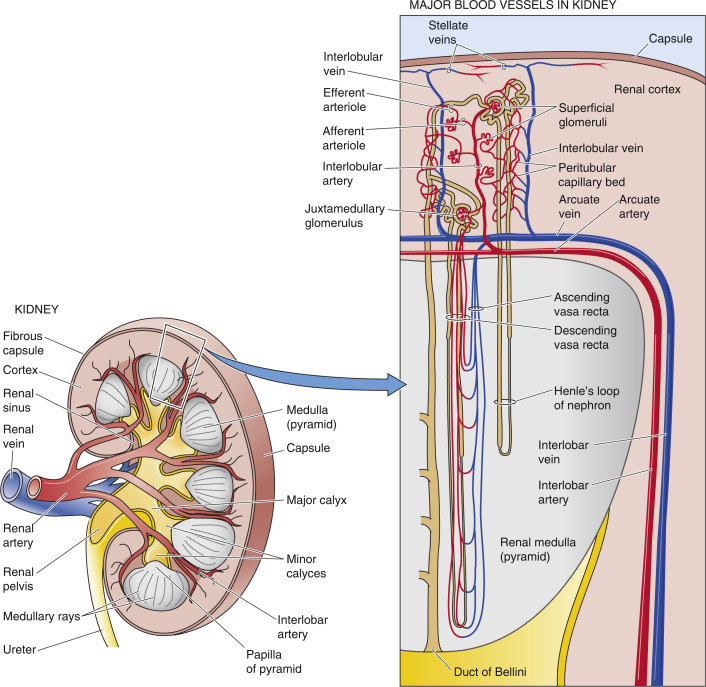
Pathophysiology
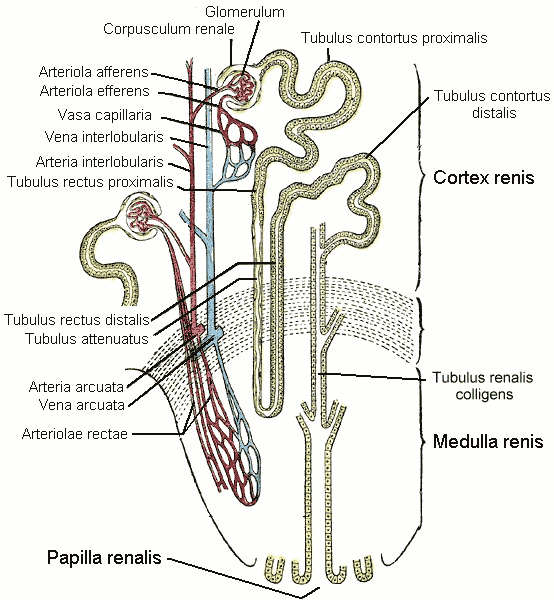
Structure of the Kidney
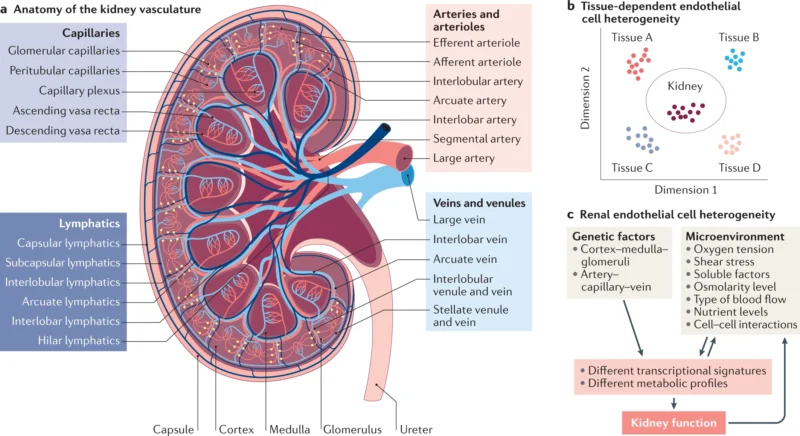
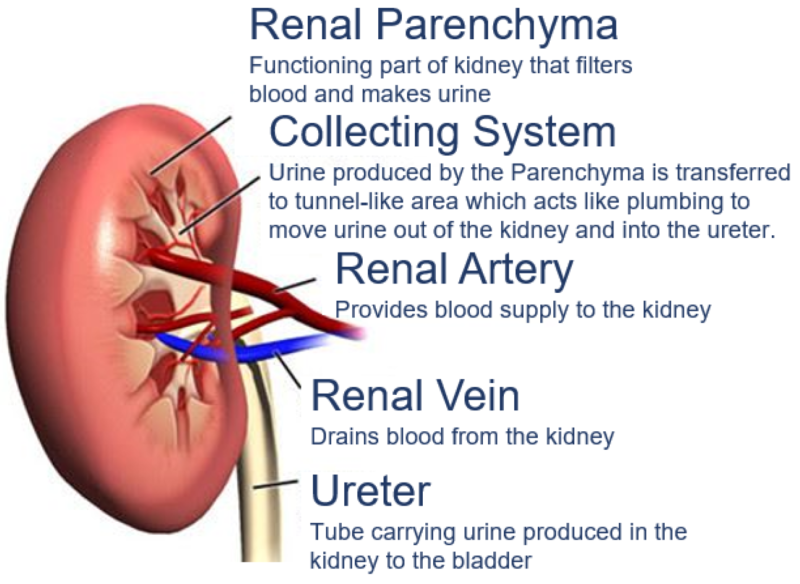
The kidneys are bean-shaped organs located on either side of the spine, just below the rib cage. Each kidney consists of two main parts:
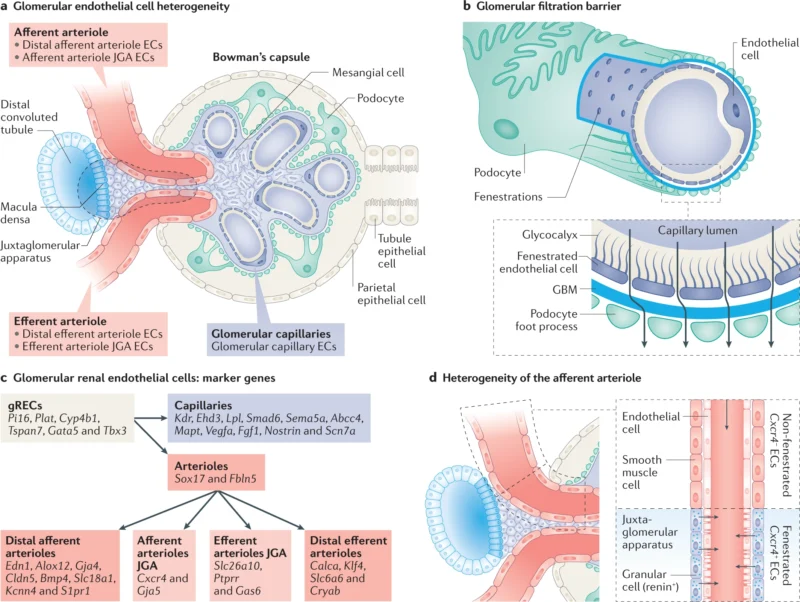
- Renal Cortex: The outer layer containing the glomeruli, where blood filtration begins.
- Renal Medulla: The inner region with structures called nephrons that concentrate urine.
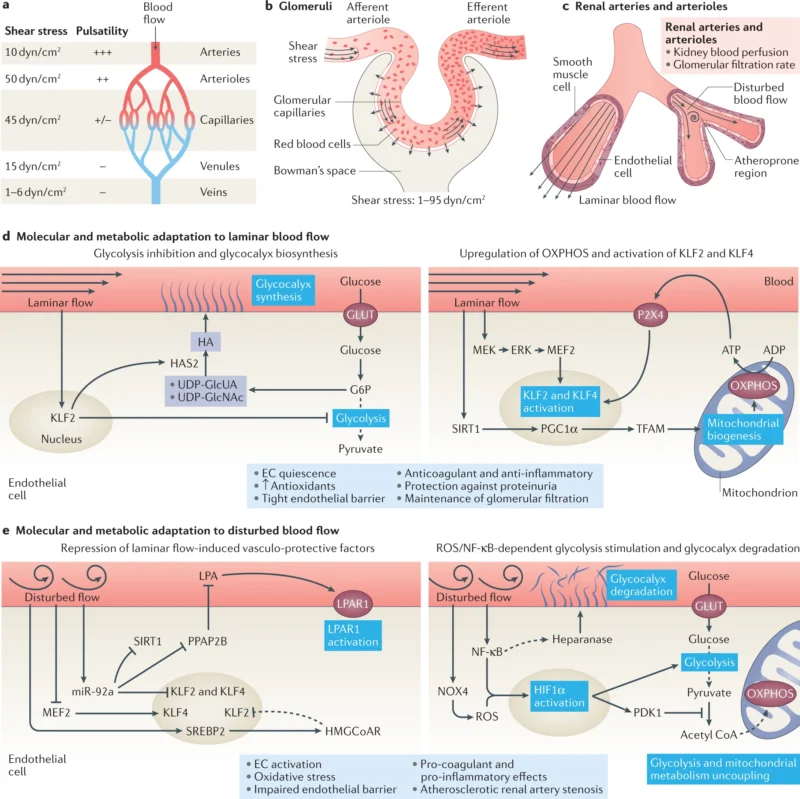
Blood Supply
Kidneys receive about 20% of the body’s blood flow through the renal arteries. Blood enters the kidneys, is filtered through the nephrons, and the filtered blood exits via the renal veins.
Nerve Supply
The kidneys are innervated by the autonomic nervous system, which regulates blood flow and filtration rates. Nerve signals help control kidney functions in response to the body’s needs.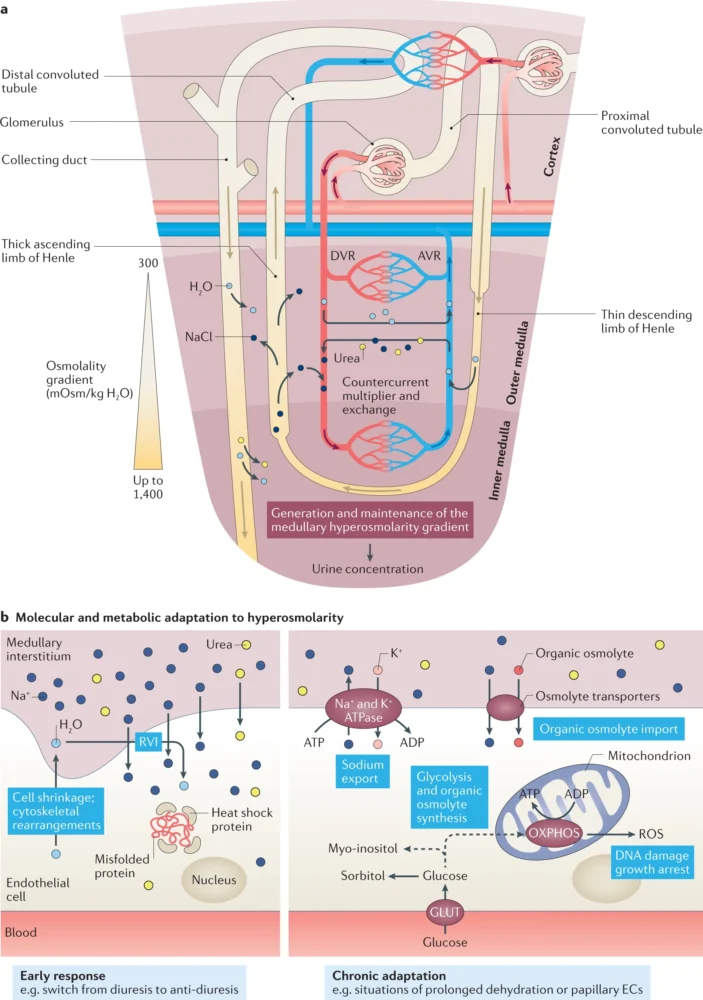
Types of Renal Parenchymal Disorders
- Glomerulonephritis: Inflammation of the glomeruli.
- Polycystic Kidney Disease: Genetic disorder causing cyst formation.
- Acute Tubular Necrosis: Damage to the kidney tubules.
- Pyelonephritis: Kidney infection.
- Interstitial Nephritis: Inflammation of the kidney’s interstitial tissue.
- Focal Segmental Glomerulosclerosis: Scarring in the glomeruli.
- Diabetic Nephropathy: Kidney damage due to diabetes.
- Hypertensive Nephrosclerosis: Kidney damage from high blood pressure.
- Alport Syndrome: Genetic condition affecting the kidneys.
- Membranous Nephropathy: Thickening of the glomerular basement membrane.
Causes
Renal parenchymal disorders can result from various factors, including:
- Infections: Such as streptococcal infections leading to post-infectious glomerulonephritis.
- Autoimmune Diseases: Like lupus affecting the kidneys.
- Genetic Mutations: Causing conditions like polycystic kidney disease.
- Diabetes: Leading to diabetic nephropathy.
- Hypertension: Chronic high blood pressure damaging kidney tissues.
- Toxins: Exposure to certain drugs or chemicals.
- Obstructions: Blockages in the urinary tract causing backpressure.
- Ischemia: Reduced blood flow to the kidneys.
- Trauma: Physical injury to the kidneys.
- Vascular Diseases: Affecting the blood vessels supplying the kidneys.
- Metabolic Disorders: Such as hypercalcemia.
- Nutritional Deficiencies: Impacting kidney health.
- Chronic Use of NSAIDs: Leading to interstitial nephritis.
- Obesity: Increasing the risk of kidney disease.
- Smoking: Contributing to kidney damage.
- Age: Older age increases susceptibility.
- Gender: Certain disorders are more common in specific genders.
- Ethnicity: Higher prevalence in some ethnic groups.
- Previous Kidney Disease: History of kidney issues.
- Environmental Factors: Exposure to heavy metals.
Symptoms
Symptoms of renal parenchymal disorders vary but may include:
- Swelling (Edema): Especially in ankles, feet, and around the eyes.
- Fatigue: Persistent tiredness.
- Decreased Urine Output: Less frequent or smaller amounts.
- Hematuria: Blood in the urine.
- Proteinuria: Excess protein in the urine.
- Hypertension: High blood pressure.
- Electrolyte Imbalances: Such as hyperkalemia.
- Anemia: Low red blood cell count.
- Back Pain: Discomfort in the kidney area.
- Nausea and Vomiting: Digestive disturbances.
- Loss of Appetite: Reduced desire to eat.
- Itching (Pruritus): Due to toxin buildup.
- Shortness of Breath: From fluid buildup in lungs.
- Confusion: Cognitive impairment.
- Muscle Cramps: From electrolyte issues.
- Dark-Colored Urine: Due to blood or proteins.
- Fever: If infection is present.
- Flank Pain: Pain in the side between the ribs and hip.
- Night Sweats: Excessive sweating at night.
- Changes in Urine Frequency: Either increased or decreased.
Diagnostic Tests
Diagnosing renal parenchymal disorders involves various tests:
- Urinalysis: Examines urine for abnormalities.
- Blood Tests: Assess kidney function (e.g., creatinine, BUN).
- Glomerular Filtration Rate (GFR): Measures kidney filtering capacity.
- Ultrasound: Visualizes kidney structure.
- CT Scan: Detailed imaging of kidneys.
- MRI: Soft tissue imaging.
- Renal Biopsy: Tissue sample analysis.
- Electrolyte Panel: Checks mineral levels.
- Blood Pressure Monitoring: Evaluates hypertension.
- Immunological Tests: Detect autoimmune markers.
- Urine Culture: Identifies infections.
- 24-Hour Urine Collection: Measures substances excreted.
- Doppler Ultrasound: Assesses blood flow.
- Nuclear Medicine Tests: Functional imaging.
- Cystoscopy: Examines the bladder and urethra.
- Kidney Function Panel: Comprehensive assessment.
- Urine Microscopy: Looks for cells and casts.
- Serum Albumin Levels: Detects protein loss.
- Metabolic Panel: Evaluates overall metabolism.
- Genetic Testing: Identifies hereditary conditions.
Non-Pharmacological Treatments
Managing renal parenchymal disorders often involves lifestyle and supportive measures:
- Dietary Modifications: Low-sodium, low-protein diets.
- Fluid Management: Adjusting fluid intake based on kidney function.
- Weight Management: Maintaining a healthy weight.
- Exercise: Regular physical activity.
- Smoking Cessation: Quitting smoking to protect kidneys.
- Limiting Alcohol: Reducing alcohol consumption.
- Blood Pressure Control: Lifestyle changes to manage hypertension.
- Blood Sugar Control: Managing diabetes through diet and exercise.
- Stress Reduction: Techniques like meditation and yoga.
- Adequate Hydration: Drinking sufficient water.
- Avoiding Nephrotoxic Substances: Steering clear of harmful chemicals.
- Regular Monitoring: Keeping track of kidney health.
- Vaccinations: Preventing infections that can harm kidneys.
- Educating Patients: Understanding the disease and management strategies.
- Support Groups: Joining communities for emotional support.
- Limiting Caffeine: Reducing caffeine intake.
- Reducing Phosphorus Intake: Managing mineral balance.
- Potassium Management: Adjusting potassium-rich foods.
- Limiting Potassium Intake: Controlling potassium levels.
- Adequate Rest: Ensuring sufficient sleep.
- Proper Hygiene: Preventing infections.
- Avoiding Over-the-Counter NSAIDs: Reducing use of pain relievers.
- Occupational Safety: Preventing workplace exposures.
- Home Blood Pressure Monitoring: Tracking hypertension.
- Limiting Dietary Phosphorus: Managing mineral balance.
- Balancing Electrolytes: Maintaining proper electrolyte levels.
- Healthy Cooking Methods: Reducing salt and unhealthy fats.
- Avoiding Excessive Protein: Preventing overburdening kidneys.
- Maintaining Regular Check-ups: Routine health evaluations.
- Implementing a Kidney-Friendly Lifestyle: Comprehensive healthy living practices.
Pharmacological Treatments
Medications play a vital role in managing renal parenchymal disorders:
- ACE Inhibitors: Lower blood pressure and reduce proteinuria.
- ARBs (Angiotensin II Receptor Blockers): Similar to ACE inhibitors.
- Diuretics: Help reduce fluid buildup.
- Beta-Blockers: Manage hypertension.
- Calcium Channel Blockers: Lower blood pressure.
- Erythropoietin: Treat anemia.
- Phosphate Binders: Control phosphorus levels.
- Vitamin D Supplements: Manage bone health.
- Insulin: Control blood sugar in diabetic patients.
- Statins: Manage cholesterol levels.
- Immunosuppressants: Treat autoimmune-related kidney diseases.
- Antibiotics: Address kidney infections.
- Anti-Inflammatory Drugs: Reduce inflammation.
- Iron Supplements: Combat anemia.
- Potassium Binders: Control potassium levels.
- Urea Cycle Modulators: Manage metabolic issues.
- Streptokinase: Break down blood clots in certain conditions.
- Calcimimetics: Manage calcium levels.
- Alkalinizing Agents: Adjust urine pH.
- Antiviral Medications: Treat viral kidney infections.
or
- ACE Inhibitors (e.g., Lisinopril)
- Angiotensin II Receptor Blockers (ARBs) (e.g., Losartan)
- Diuretics (e.g., Furosemide)
- Beta-Blockers (e.g., Metoprolol)
- Calcium Channel Blockers (e.g., Amlodipine)
- Erythropoiesis-Stimulating Agents (e.g., Epoetin alfa)
- Phosphate Binders (e.g., Sevelamer)
- Vitamin D Analogues (e.g., Calcitriol)
- SGLT2 Inhibitors (e.g., Canagliflozin)
- Immunosuppressants (e.g., Prednisone)
- Antibiotics (e.g., Ciprofloxacin for infections)
- Statins (e.g., Atorvastatin)
- Iron Supplements (e.g., Ferrous sulfate)
- Potassium Binders (e.g., Kayexalate)
- Alkalinizing Agents (e.g., Sodium bicarbonate)
- Antihyperglycemics (e.g., Insulin)
- Anticoagulants (e.g., Warfarin)
- Proton Pump Inhibitors (e.g., Omeprazole)
- Antihistamines (for itching)
- Analgesics (e.g., Acetaminophen)
Surgical Interventions
In severe cases, surgery may be necessary:
- Nephrectomy: Removal of part or all of a kidney.
- Kidney Transplant: Replacing a diseased kidney with a healthy one.
- Dialysis Access Surgery: Creating vascular access for dialysis.
- Ureteral Stent Placement: Relieving urinary obstructions.
- Renal Artery Stenting: Opening narrowed blood vessels.
- Pyeloplasty: Correcting ureteropelvic junction obstruction.
- Partial Nephrectomy: Removing a tumor while preserving kidney tissue.
- Percutaneous Nephrolithotomy: Removing large kidney stones.
- Biopsy Procedures: Surgically obtaining kidney tissue samples.
- Vascular Bypass Surgery: Improving blood flow to kidneys.
Prevention Strategies
Preventing renal parenchymal disorders involves:
- Maintaining Healthy Blood Pressure: Regular monitoring and management.
- Controlling Blood Sugar Levels: Managing diabetes effectively.
- Healthy Diet: Balanced, low-sodium, and low-protein intake.
- Regular Exercise: Promoting overall health.
- Avoiding Smoking: Reducing risk factors for kidney disease.
- Limiting Alcohol Consumption: Protecting kidney function.
- Staying Hydrated: Ensuring adequate fluid intake.
- Avoiding Excessive Use of NSAIDs: Preventing kidney damage from medications.
- Regular Health Screenings: Early detection of kidney issues.
- Managing Weight: Preventing obesity-related kidney problems.
When to See a Doctor
Seek medical attention if you experience:
- Persistent Swelling: In ankles, feet, or around the eyes.
- Unexplained Fatigue: Constant tiredness without reason.
- Changes in Urination: Frequency, color, or amount.
- Pain in the Back or Side: Near the kidneys.
- High Blood Pressure: Especially if uncontrolled.
- Blood in Urine: Visible or detected via tests.
- Persistent Fever: Accompanied by other symptoms.
- Nausea and Vomiting: Without clear cause.
- Shortness of Breath: Linked to kidney issues.
- Itching or Rashes: Without obvious skin conditions.
- Confusion or Difficulty Concentrating: Cognitive changes.
- Muscle Cramps: Unexplained muscle pain.
- Loss of Appetite: Significant weight loss.
- Weakness: Generalized muscle weakness.
- Night Sweats: Excessive sweating during sleep.
Frequently Asked Questions (FAQs)
- What are renal parenchymal disorders?
- Conditions affecting the functional tissue of the kidneys, impacting their ability to filter blood and maintain bodily functions.
- What causes glomerulonephritis?
- It can be caused by infections, autoimmune diseases, or other inflammatory conditions.
- How is polycystic kidney disease inherited?
- It is usually inherited in an autosomal dominant pattern, meaning one parent can pass it to their child.
- Can renal parenchymal disorders be cured?
- While some conditions can be managed effectively, others may lead to chronic kidney disease requiring ongoing treatment.
- What is the role of dialysis in kidney disease?
- Dialysis performs the kidneys’ filtering functions when they are no longer able to work adequately.
- How does high blood pressure affect the kidneys?
- It damages blood vessels in the kidneys, reducing their ability to function properly.
- Are renal parenchymal disorders preventable?
- Many can be prevented through healthy lifestyle choices and managing underlying conditions like diabetes and hypertension.
- What dietary changes help manage kidney disease?
- Reducing salt, protein, and phosphorus intake can alleviate kidney strain.
- Is kidney transplantation the only surgical option?
- Transplantation is a common option, but other surgeries may address specific issues like obstructions or tumors.
- Can children develop renal parenchymal disorders?
- Yes, some disorders like congenital abnormalities and genetic conditions can affect children.
- What lifestyle changes support kidney health?
- Maintaining a healthy weight, exercising regularly, and avoiding smoking and excessive alcohol.
- How often should kidney function be tested?
- Individuals at risk should have regular check-ups as advised by their healthcare provider, typically annually.
- What is the prognosis for renal parenchymal disorders?
- It varies depending on the specific disorder, its severity, and how early it is detected and treated.
- Can herbal supplements harm the kidneys?
- Some supplements can be nephrotoxic; it’s essential to consult a doctor before use.
- What is the difference between acute and chronic kidney disease?
- Acute kidney disease is sudden and often reversible, while chronic kidney disease develops over time and is usually irreversible.
Conclusion
Renal parenchymal disorders encompass a wide range of kidney conditions that can significantly impact overall health. Early detection, effective management, and preventive measures are crucial in mitigating the adverse effects of these disorders. Maintaining a healthy lifestyle, regular medical check-ups, and adhering to prescribed treatments can help preserve kidney function and enhance quality of life.
Disclaimer: Each person’s journey is unique, treatment plan, life style, food habit, hormonal condition, immune system, chronic disease condition, geological location, weather and previous medical history is also unique. So always seek the best advice from a qualified medical professional or health care provider before trying any treatments to ensure to find out the best plan for you. This guide is for general information and educational purposes only. Regular check-ups and awareness can help to manage and prevent complications associated with these diseases conditions. If you or someone are suffering from this disease condition bookmark this website or share with someone who might find it useful! Boost your knowledge and stay ahead in your health journey. We always try to ensure that the content is regularly updated to reflect the latest medical research and treatment options. Thank you for giving your valuable time to read the article.