The renal corticomedullary junction (CMJ) is the area in the kidney where the outer cortex meets the inner medulla. Disorders in this region can impact kidney function, affecting overall health. This article will explore the pathophysiology, types, causes, symptoms, diagnostic tests, treatments, and when to seek medical attention.
Pathophysiology
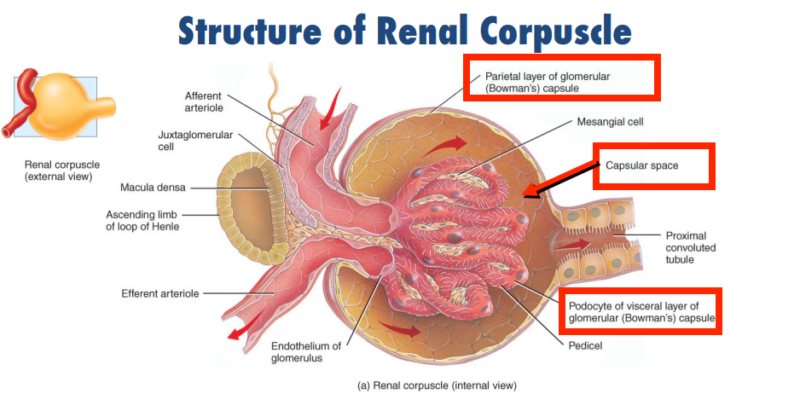
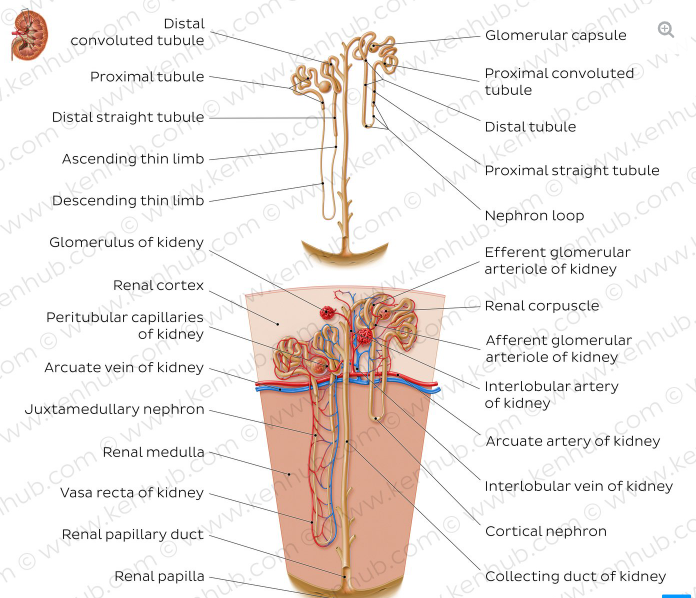
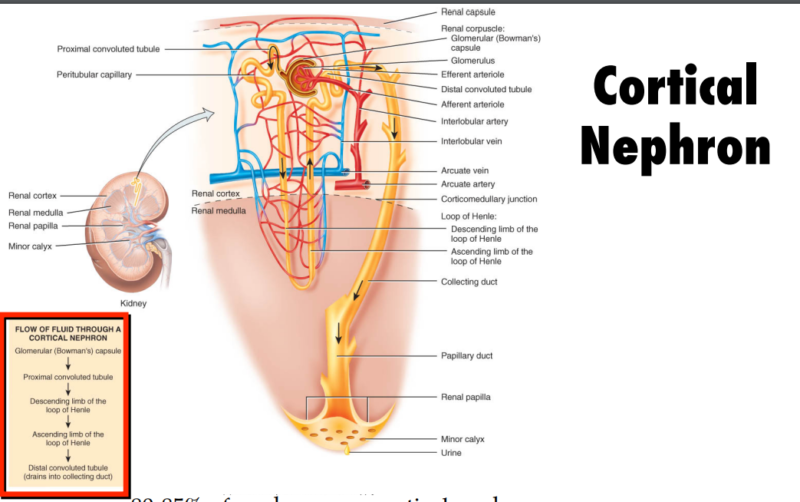
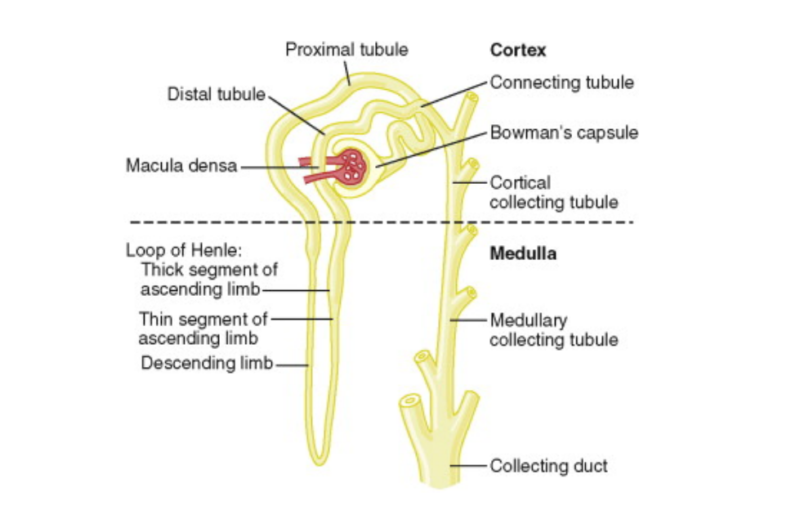
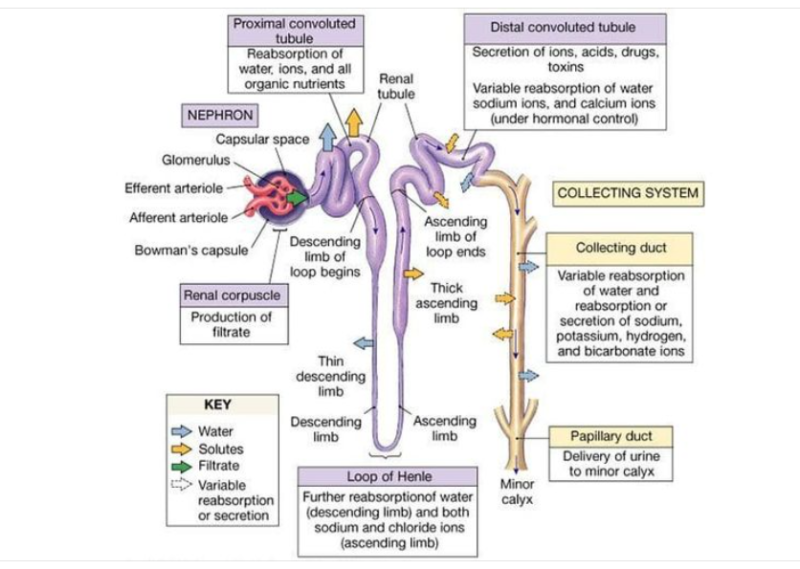
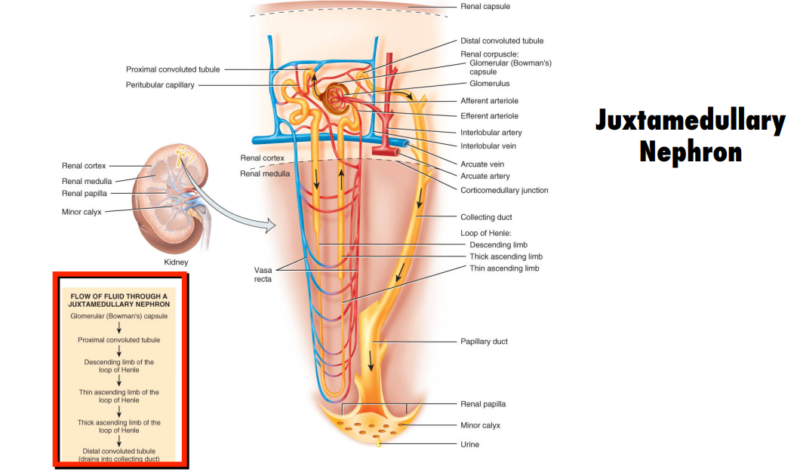
Structure
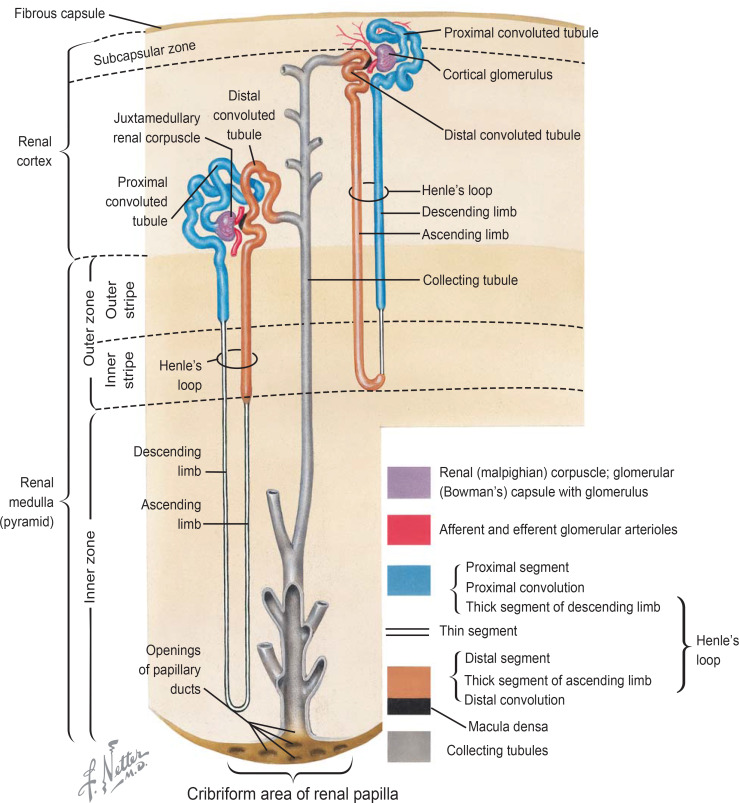
The kidney consists of several parts:
- Cortex: The outer layer where blood filtration begins.
- Medulla: The inner layer responsible for urine concentration.
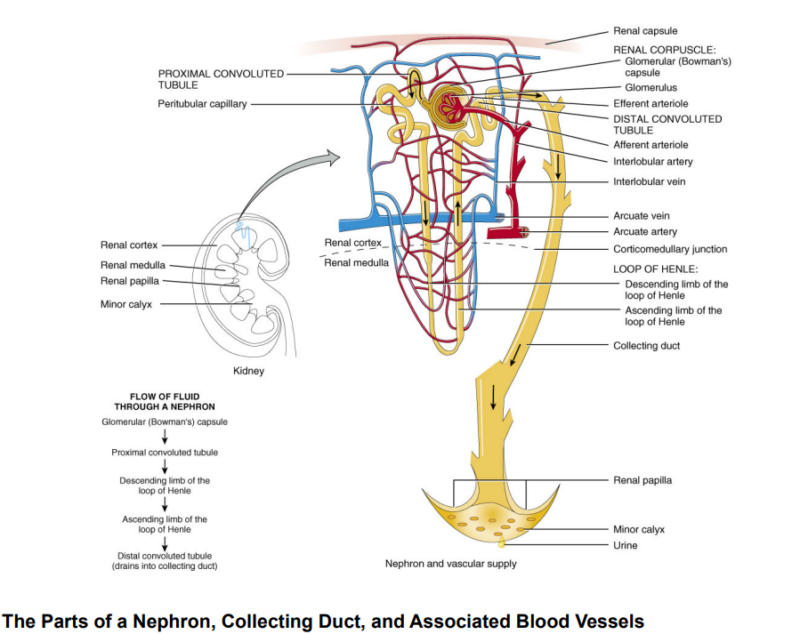
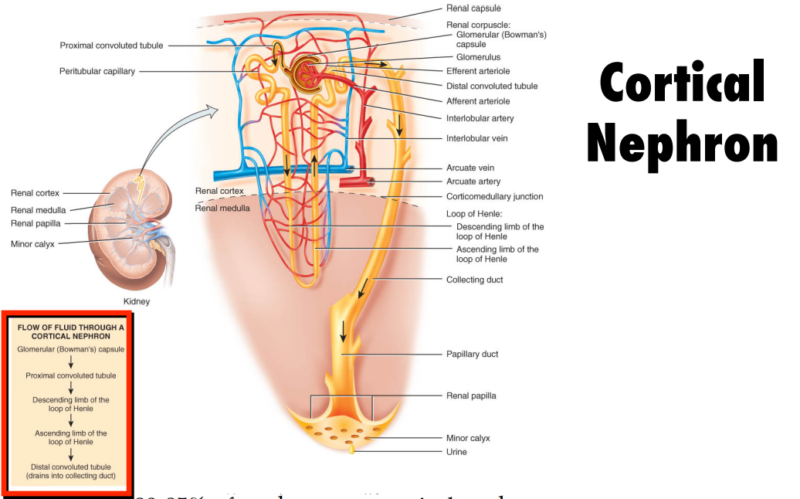
- Corticomedullary Junction (CMJ): The boundary between the cortex and medulla, playing a crucial role in kidney function.
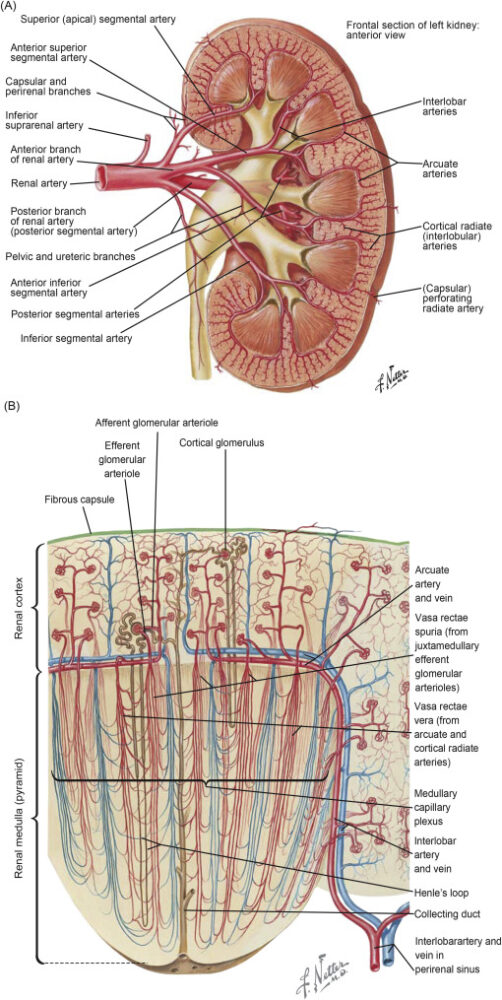
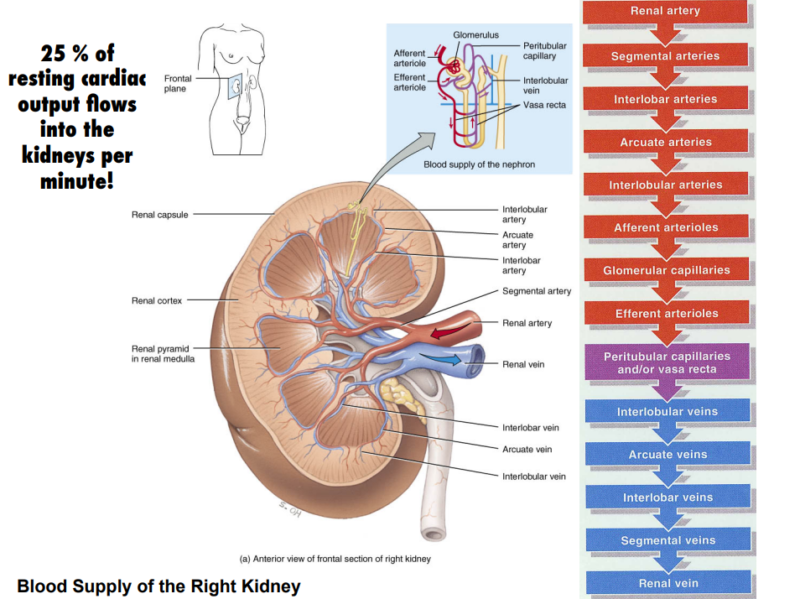
Blood Supply
The renal arteries supply blood to the kidneys, branching into smaller arterioles and capillaries within the cortex and medulla. This blood flow is essential for filtering waste and regulating blood pressure.
Nerve Supply
The kidneys receive nerves from the autonomic nervous system, which helps control kidney functions like blood flow and filtration.
Types of Renal Corticomedullary Junction Disorders
- Acute Kidney Injury (AKI)
- Chronic Kidney Disease (CKD)
- Renal Vascular Disorders
- Interstitial Nephritis
- Cystic Kidney Diseases
- Diabetic Nephropathy
- Renal Cell Carcinoma
- Ureteropelvic Junction Obstruction
- Medullary Sponge Kidney
- Papillary Necrosis
Causes of Renal Corticomedullary Junction Disorders
- Diabetes
- Hypertension
- Infections
- Autoimmune Diseases
- Toxins
- Medications
- Genetic Conditions
- Obstruction of Urinary Tract
- Kidney Stones
- Ischemia
- Trauma
- Dehydration
- Pregnancy-related changes
- Chronic Inflammation
- High Protein Diets
- Hypercalcemia
- Polycystic Kidney Disease
- Vascular Malformations
- Obesity
- Smoking
Symptoms of Renal Corticomedullary Junction Disorders
- Fatigue
- Swelling (Edema)
- Nausea
- Vomiting
- Decreased Urine Output
- High Blood Pressure
- Anemia
- Confusion
- Back Pain
- Itching
- Muscle Cramps
- Shortness of Breath
- Foul-smelling urine
- Foamy urine
- Weight loss
- Fluid retention
- Bloating
- Pale skin
- Dry mouth
- Difficulty concentrating
Diagnostic Tests
- Blood Tests (Creatinine, BUN)
- Urinalysis
- Ultrasound
- CT Scan
- MRI
- Kidney Biopsy
- 24-hour Urine Collection
- Radionuclide Scan
- X-rays
- Electrolyte Tests
- Glomerular Filtration Rate (GFR) Test
- Urine Culture
- Renal Angiography
- Cystoscopy
- Stool Tests for Blood
- Liver Function Tests
- Genetic Testing
- Serum Albumin Test
- Hydration Tests
- Blood Gas Analysis
Non-Pharmacological Treatments
- Dietary Changes
- Hydration
- Regular Exercise
- Weight Management
- Stress Reduction Techniques
- Smoking Cessation
- Limiting Alcohol Intake
- Regular Health Check-ups
- Dialysis (if severe)
- Avoiding Over-the-Counter NSAIDs
- Managing Blood Sugar Levels
- Monitoring Blood Pressure
- Limiting Sodium Intake
- Increasing Potassium Intake (as advised)
- Using Herbal Remedies (with caution)
- Participating in Support Groups
- Educating Yourself about the Disease
- Engaging in Mindfulness Practices
- Massage Therapy
- Acupuncture
Medications
- ACE Inhibitors
- ARBs (Angiotensin Receptor Blockers)
- Diuretics
- Antibiotics (for infections)
- Immunosuppressants
- Pain Relief Medications
- Phosphate Binders
- Erythropoiesis-Stimulating Agents
- Vitamin D Supplements
- Statins
- Glucose-Lowering Drugs
- Anti-hypertensives
- Corticosteroids
- Antihistamines (for itching)
- Antacids
- Calcium Supplements
- Folic Acid
- Omega-3 Fatty Acids
- Potassium-sparing Diuretics
- Antidepressants (for mental health)
Surgical Options
- Kidney Transplant
- Nephrectomy (kidney removal)
- Ureteral Stenting
- Balloon Angioplasty
- Surgical Correction of Urinary Tract Obstructions
- Resection of Tumors
- Renal Artery Bypass
- Cyst Removal
- Ureterectomy
- Endoscopic Procedures for Stones
Prevention Strategies
- Maintain Healthy Blood Pressure
- Control Blood Sugar Levels
- Stay Hydrated
- Eat a Balanced Diet
- Avoid Excessive Alcohol
- Quit Smoking
- Regular Exercise
- Limit NSAID Use
- Routine Health Screenings
- Educate Yourself on Kidney Health
- Monitor Cholesterol Levels
- Manage Stress
- Stay Active
- Follow Doctor’s Recommendations
- Limit Processed Foods
- Maintain Healthy Weight
- Control Blood Lipids
- Ensure Safe Use of Supplements
- Practice Safe Sex
- Avoid Dehydration
When to See a Doctor
- Persistent fatigue or weakness
- Sudden changes in urine output
- Swelling in legs or face
- Severe back or flank pain
- Blood in urine
- Unexplained weight loss
- Nausea or vomiting that doesn’t improve
- Difficulty breathing
- High blood pressure that’s hard to control
- Changes in appetite or taste
Frequently Asked Questions (FAQs)
- What is the corticomedullary junction?
- It’s the area where the kidney’s outer and inner layers meet.
- What causes disorders in this area?
- Causes include diabetes, hypertension, infections, and genetic conditions.
- What are common symptoms?
- Symptoms may include fatigue, swelling, nausea, and decreased urine output.
- How are these disorders diagnosed?
- Diagnosis involves blood tests, urinalysis, imaging, and sometimes biopsy.
- What treatments are available?
- Treatments can include medications, dietary changes, and sometimes surgery.
- Can these disorders be prevented?
- Yes, by managing risk factors like diabetes and hypertension.
- When should I see a doctor?
- If you experience severe symptoms like swelling or significant changes in urine output.
- Are there specific diets for kidney health?
- Yes, a balanced diet low in salt and protein is often recommended.
- Can stress affect kidney health?
- Yes, chronic stress can impact overall health, including kidney function.
- Is kidney disease reversible?
- Some conditions may be reversible with prompt treatment, while others may lead to chronic issues.
- What lifestyle changes can help?
- Staying hydrated, exercising, and eating a balanced diet can significantly improve kidney health.
- Are there support groups for kidney disorders?
- Yes, many organizations offer resources and community support.
- How often should I get my kidneys checked?
- It varies, but regular check-ups are advisable, especially if you have risk factors.
- Do I need to change my medications?
- Always consult your doctor before making any changes to your medication regimen.
- Can herbal remedies help with kidney disorders?
- Some may help, but it’s essential to discuss any herbal treatments with your doctor.
Conclusion
Understanding renal corticomedullary junction disorders is crucial for early detection and treatment. If you experience any concerning symptoms, consult a healthcare provider for evaluation and management. Early intervention can make a significant difference in kidney health and overall well-being.
Disclaimer: Each person’s journey is unique, treatment plan, life style, food habit, hormonal condition, immune system, chronic disease condition, geological location, weather and previous medical history is also unique. So always seek the best advice from a qualified medical professional or health care provider before trying any treatments to ensure to find out the best plan for you. This guide is for general information and educational purposes only. Regular check-ups and awareness can help to manage and prevent complications associated with these diseases conditions. If you or someone are suffering from this disease condition bookmark this website or share with someone who might find it useful! Boost your knowledge and stay ahead in your health journey. We always try to ensure that the content is regularly updated to reflect the latest medical research and treatment options. Thank you for giving your valuable time to read the article.



