Connecting Tubule Obstruction is a condition that affects the kidneys, specifically the connecting tubules within the nephron—the functional unit of the kidney. This article provides an in-depth look into what connecting tubule obstruction is, its causes, symptoms, diagnostic methods, treatments, prevention strategies, and more. Whether you’re seeking information for personal knowledge or to support a loved one, this guide offers clear and accessible insights.
The connecting tubule is a part of the nephron in the kidney that plays a crucial role in regulating the body’s fluid and electrolyte balance. Connecting tubule obstruction occurs when there is a blockage in these tubules, hindering the normal flow of urine. This obstruction can lead to various kidney dysfunctions, impacting overall health.
Pathophysiology
Understanding the pathophysiology of connecting tubule obstruction involves looking at the structure, blood supply, and nerve supply of the connecting tubules.
Structure
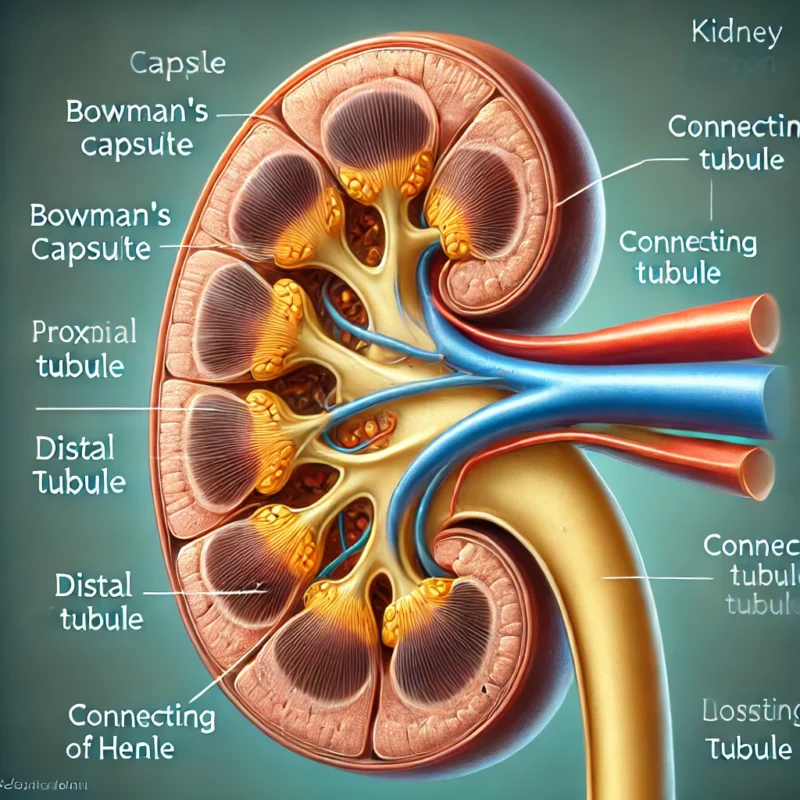
The nephron consists of several parts: the glomerulus, proximal tubule, loop of Henle, distal tubule, connecting tubule, and collecting duct. The connecting tubule links the distal tubule to the collecting duct, facilitating the final adjustments in urine composition.
Blood Supply
The kidneys receive blood through the renal arteries, which branch into smaller arterioles supplying each part of the nephron. Proper blood flow is essential for the kidneys to filter blood and produce urine.
Nerve Supply
The kidneys are innervated by the autonomic nervous system, which regulates blood flow and kidney function. Nerve signals help control the constriction and dilation of blood vessels within the kidneys.
Types of Connecting Tubule Obstruction
Connecting tubule obstruction can be classified based on the location and cause of the blockage:
- Mechanical Obstruction: Physical blockage due to stones, tumors, or cysts.
- Functional Obstruction: Issues related to the function of the tubule cells, such as fibrosis or inflammation.
- Chemical Obstruction: Caused by substances that interfere with tubule function, like certain drugs or toxins.
Causes
Here are 20 potential causes of connecting tubule obstruction:
- Kidney Stones: Solid mineral deposits blocking the tubules.
- Tumors: Growths in the kidneys causing blockages.
- Cysts: Fluid-filled sacs that can obstruct tubules.
- Fibrosis: Scarring that narrows or blocks tubules.
- Infections: Inflammation from bacterial or viral infections.
- Autoimmune Diseases: Conditions like lupus affecting kidney function.
- Polycystic Kidney Disease: Genetic disorder causing multiple cysts.
- Obstructive Uropathy: Blockage in the urinary tract affecting the kidneys.
- Medications: Certain drugs causing tubule damage.
- Toxins: Exposure to harmful chemicals affecting kidney function.
- Dehydration: Severe lack of fluids impacting urine flow.
- Hypertension: High blood pressure damaging kidney structures.
- Diabetes: High blood sugar leading to kidney damage.
- Glomerulonephritis: Inflammation of the glomeruli affecting tubules.
- Pyelonephritis: Severe kidney infection causing obstruction.
- Ureteral Strictures: Narrowing of the ureters affecting urine flow.
- Congenital Abnormalities: Birth defects impacting kidney structure.
- Lithiasis: Formation of stones within the kidney.
- Radiation Therapy: Treatment causing kidney damage.
- Surgical Complications: Procedures leading to kidney obstruction.
Symptoms
Recognizing the symptoms of connecting tubule obstruction is crucial for early diagnosis and treatment. Here are 20 possible symptoms:
- Flank Pain: Sharp pain in the side or back.
- Hematuria: Blood in the urine.
- Frequent Urination: Needing to urinate more often.
- Painful Urination: Discomfort during urination.
- Urine Changes: Cloudy or foul-smelling urine.
- Swelling: Edema in legs, ankles, or face.
- High Blood Pressure: Elevated blood pressure levels.
- Fatigue: Persistent tiredness.
- Nausea: Feeling sick to the stomach.
- Vomiting: Actual vomiting episodes.
- Fever: Elevated body temperature.
- Chills: Shivering or feeling cold.
- Loss of Appetite: Reduced desire to eat.
- Back Pain: Pain in the lower back region.
- Electrolyte Imbalance: Irregular levels of minerals in the blood.
- Anemia: Low red blood cell count causing weakness.
- Shortness of Breath: Difficulty breathing.
- Confusion: Mental fog or difficulty concentrating.
- Decreased Urine Output: Producing less urine than usual.
- Metallic Taste: Unusual taste in the mouth.
Diagnostic Tests
Diagnosing connecting tubule obstruction involves various tests to assess kidney function and identify the blockage. Here are 20 diagnostic tests:
- Urinalysis: Examines the composition of urine.
- Blood Tests: Measures kidney function markers like creatinine.
- Ultrasound: Uses sound waves to visualize the kidneys.
- CT Scan: Detailed imaging to detect obstructions.
- MRI: Magnetic imaging for soft tissue assessment.
- Intravenous Pyelogram (IVP): X-ray after injecting dye to view urine flow.
- Renal Scintigraphy: Nuclear imaging of kidney function.
- Cystoscopy: Endoscopic examination of the bladder and urethra.
- Biopsy: Sampling kidney tissue for microscopic analysis.
- Electrolyte Panel: Checks mineral levels in the blood.
- Glomerular Filtration Rate (GFR): Measures kidney filtering capacity.
- Urodynamic Tests: Assess bladder and urethra function.
- KUB X-ray: Imaging of the kidneys, ureters, and bladder.
- DMSA Scan: Nuclear scan for kidney scarring.
- Venous Renal Pressure Measurement: Checks pressure within kidney veins.
- Arteriography: Imaging of kidney blood vessels.
- Ureteroscopy: Endoscopic examination of the ureters.
- PVR Measurement (Post-Void Residual): Amount of urine left after urination.
- Electrocardiogram (ECG): Evaluates heart function related to kidney issues.
- Urine Culture: Detects infections causing obstruction.
Non-Pharmacological Treatments
Managing connecting tubule obstruction often involves lifestyle changes and other non-drug approaches. Here are 30 non-pharmacological treatments:
- Hydration: Drinking plenty of water to flush kidneys.
- Dietary Changes: Low-sodium, low-protein diets to reduce kidney strain.
- Weight Management: Maintaining a healthy weight to lower risk.
- Exercise: Regular physical activity to improve overall health.
- Quit Smoking: Reducing kidney damage from tobacco use.
- Limit Alcohol: Reducing alcohol intake to protect kidneys.
- Stress Reduction: Techniques like meditation and yoga.
- Adequate Rest: Ensuring sufficient sleep for recovery.
- Avoiding Toxins: Steering clear of harmful chemicals.
- Regular Monitoring: Keeping track of kidney function.
- Low-Potassium Diet: Managing electrolyte levels.
- Low-Phosphorus Diet: Reducing phosphorus intake.
- Blood Pressure Control: Lifestyle changes to manage hypertension.
- Blood Sugar Control: Managing diabetes through diet and exercise.
- Limit Caffeine: Reducing caffeine to lower kidney stress.
- Natural Diuretics: Foods like watermelon to promote urine flow.
- Herbal Supplements: Using safe herbs under supervision.
- Acupuncture: Alternative therapy to alleviate symptoms.
- Massage Therapy: Relieving muscle tension and pain.
- Physical Therapy: Improving mobility and reducing pain.
- Compression Stockings: Managing swelling in legs.
- Dietary Fiber: Aiding digestion and kidney health.
- Avoiding NSAIDs: Reducing use of nonsteroidal anti-inflammatory drugs.
- Healthy Fats: Incorporating omega-3 fatty acids.
- Limit Red Meat: Reducing intake to lower kidney burden.
- Plant-Based Diet: Emphasizing vegetables and grains.
- Probiotics: Supporting gut health, indirectly benefiting kidneys.
- Regular Check-ups: Visiting healthcare providers routinely.
- Education: Learning about kidney health and management.
- Support Groups: Connecting with others for emotional support.
Medications
While non-pharmacological treatments are essential, medications may also be necessary. Here are 20 drugs commonly used in managing connecting tubule obstruction:
- Diuretics: Help increase urine production.
- ACE Inhibitors: Lower blood pressure and protect kidney function.
- ARBs (Angiotensin II Receptor Blockers): Similar to ACE inhibitors.
- Beta-Blockers: Manage high blood pressure.
- Calcium Channel Blockers: Control hypertension.
- Antibiotics: Treat kidney infections causing obstruction.
- Pain Relievers: Manage pain without harming kidneys.
- Phosphate Binders: Control phosphorus levels in the blood.
- Erythropoietin: Treat anemia related to kidney disease.
- Vitamin D Supplements: Support bone health affected by kidney issues.
- Sodium Bicarbonate: Manage metabolic acidosis.
- Insulin: Control blood sugar in diabetic patients.
- Statins: Lower cholesterol to reduce cardiovascular risk.
- Iron Supplements: Address iron deficiency anemia.
- Potassium Binders: Manage high potassium levels.
- Alkali Agents: Correct electrolyte imbalances.
- Immunosuppressants: Treat autoimmune-related kidney damage.
- Urate-Lowering Drugs: Manage gout affecting kidneys.
- Anticoagulants: Prevent blood clots in certain conditions.
- Natriuretic Peptides: Promote sodium excretion.
Surgical Treatments
In severe cases, surgery may be required to remove obstructions or repair damaged kidney structures. Here are 10 surgical options:
- Nephrolithotomy: Removal of large kidney stones.
- Ureteroscopy: Endoscopic procedure to remove obstructions in the ureters.
- Percutaneous Nephrostomy: Drainage of urine from the kidney.
- Pyeloplasty: Repairing the renal pelvis to relieve obstruction.
- Transurethral Resection: Removing parts of the urinary tract causing blockage.
- Kidney Transplant: Replacing a diseased kidney with a healthy one.
- Lithotripsy: Breaking down stones using shock waves.
- Cystectomy: Removal of the bladder if severely affected.
- Renal Denervation: Disrupting nerves to reduce blood pressure.
- Ureteral Stenting: Inserting a tube to keep the ureter open.
Prevention
Preventing connecting tubule obstruction involves maintaining overall kidney health and addressing risk factors. Here are 10 prevention strategies:
- Stay Hydrated: Drink plenty of water daily.
- Healthy Diet: Eat a balanced diet low in salt and protein.
- Regular Exercise: Maintain a healthy weight through physical activity.
- Control Blood Pressure: Monitor and manage hypertension.
- Manage Diabetes: Keep blood sugar levels in check.
- Avoid Smoking: Reduce risk of kidney damage.
- Limit Alcohol Intake: Keep alcohol consumption moderate.
- Avoid Excessive NSAIDs: Use pain relievers responsibly.
- Regular Medical Check-ups: Early detection of kidney issues.
- Protect Against Infections: Practice good hygiene to prevent kidney infections.
When to See a Doctor
Seek medical attention if you experience any of the following:
- Severe or persistent flank or back pain.
- Blood in your urine.
- Frequent, painful, or difficult urination.
- Unexplained swelling in your legs, ankles, or face.
- High blood pressure not controlled by medication.
- Persistent fatigue or weakness.
- Signs of infection, such as fever and chills.
- Sudden changes in urine output.
- Nausea or vomiting without an apparent cause.
- Any other unusual symptoms related to kidney function.
Frequently Asked Questions (FAQs)
- What is the connecting tubule?
- It’s a part of the nephron in the kidney that helps regulate urine composition.
- What causes connecting tubule obstruction?
- Causes include kidney stones, tumors, cysts, infections, and certain diseases.
- Can connecting tubule obstruction be cured?
- Many cases can be treated effectively with medications, lifestyle changes, or surgery.
- Is connecting tubule obstruction a common condition?
- It’s less common than other kidney issues but still significant in affecting kidney function.
- What are the risks if left untreated?
- Potential kidney damage, high blood pressure, electrolyte imbalances, and kidney failure.
- How is connecting tubule obstruction diagnosed?
- Through tests like urinalysis, blood tests, imaging studies, and sometimes biopsy.
- Can lifestyle changes help manage the condition?
- Yes, staying hydrated, maintaining a healthy diet, and controlling blood pressure are beneficial.
- Are there any dietary restrictions?
- Depending on the cause, you may need to limit salt, protein, potassium, or phosphorus.
- Is surgery always required for obstruction?
- Not always; many cases can be managed with less invasive treatments.
- Can connecting tubule obstruction lead to kidney failure?
- Yes, especially if not treated promptly and effectively.
- Who is at risk for this condition?
- Individuals with a history of kidney stones, certain genetic conditions, diabetes, or high blood pressure.
- Can children develop connecting tubule obstruction?
- Yes, although it’s less common, especially in cases of congenital abnormalities.
- Is there a genetic component to the condition?
- Some causes, like polycystic kidney disease, have a genetic basis.
- How long does treatment take?
- It varies based on the cause and severity but can range from weeks to months.
- Can connecting tubule obstruction recur?
- Yes, especially if underlying risk factors are not managed.
Conclusion
Connecting Tubule Obstruction is a serious kidney condition that requires timely diagnosis and appropriate treatment. Understanding its causes, symptoms, and available treatments can empower you to take proactive steps in managing kidney health. If you suspect any issues related to kidney function, consult a healthcare professional promptly to ensure the best possible outcomes.
Disclaimer: Each person’s journey is unique, treatment plan, life style, food habit, hormonal condition, immune system, chronic disease condition, geological location, weather and previous medical history is also unique. So always seek the best advice from a qualified medical professional or health care provider before trying any treatments to ensure to find out the best plan for you. This guide is for general information and educational purposes only. Regular check-ups and awareness can help to manage and prevent complications associated with these diseases conditions. If you or someone are suffering from this disease condition bookmark this website or share with someone who might find it useful! Boost your knowledge and stay ahead in your health journey. We always try to ensure that the content is regularly updated to reflect the latest medical research and treatment options. Thank you for giving your valuable time to read the article.



