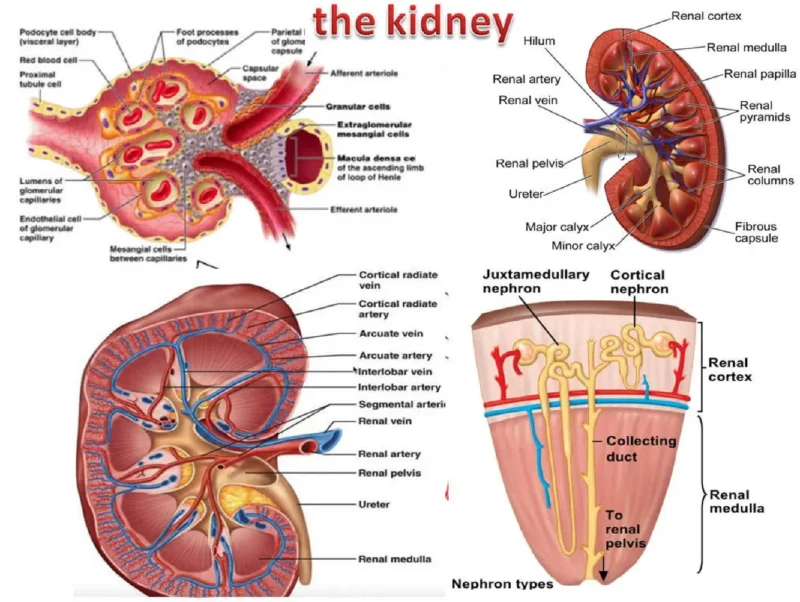
The ascending vasa recta are small blood vessels in the kidney that play a crucial role in maintaining blood flow and the body’s balance of fluids and electrolytes. Disorders affecting these vessels can lead to significant health issues.
Pathophysiology
Structure
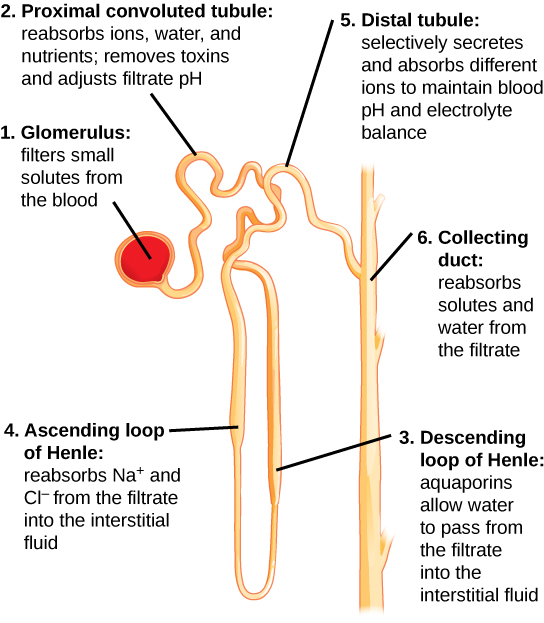
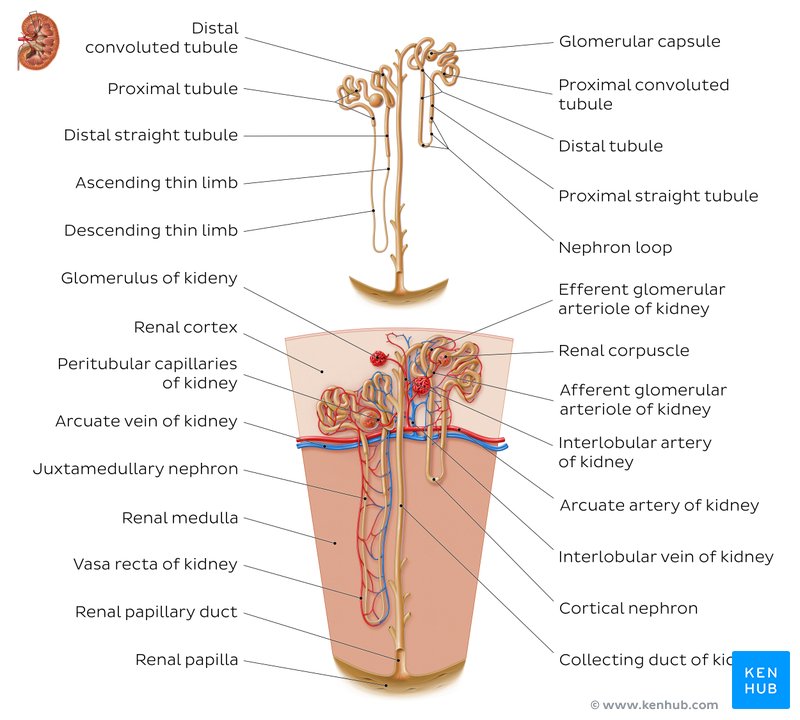
The ascending vasa recta are part of the renal blood supply. They branch off from the renal artery and travel alongside the loops of Henle in the nephron.
Blood Supply
These vessels supply blood to the medulla of the kidney, which is essential for the kidney’s ability to concentrate urine.
Nerve Supply
The nerves that innervate the vasa recta come from the autonomic nervous system, helping to regulate blood flow according to the body’s needs.
Types of Ascending Vasa Recta Disorders
- Ischemic Disorders: Reduced blood flow causing tissue damage.
- Inflammatory Disorders: Inflammation of the vasa recta, leading to various symptoms.
- Congenital Disorders: Abnormal development of the vasa recta.
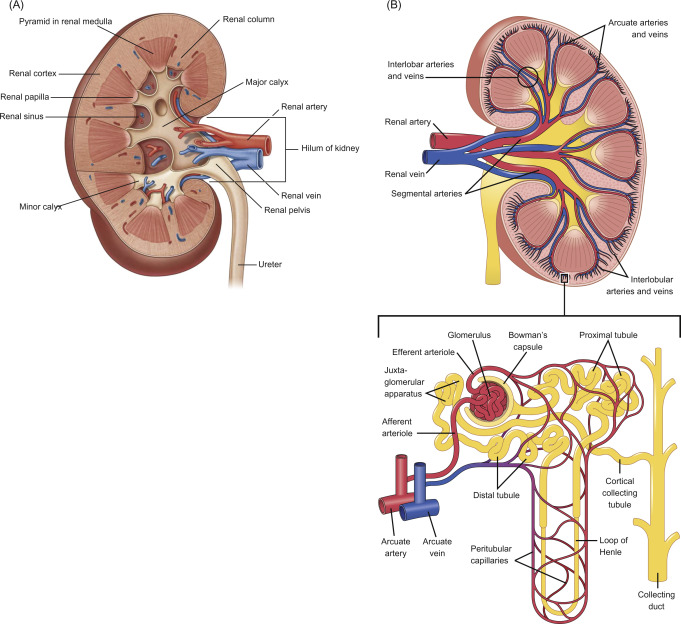
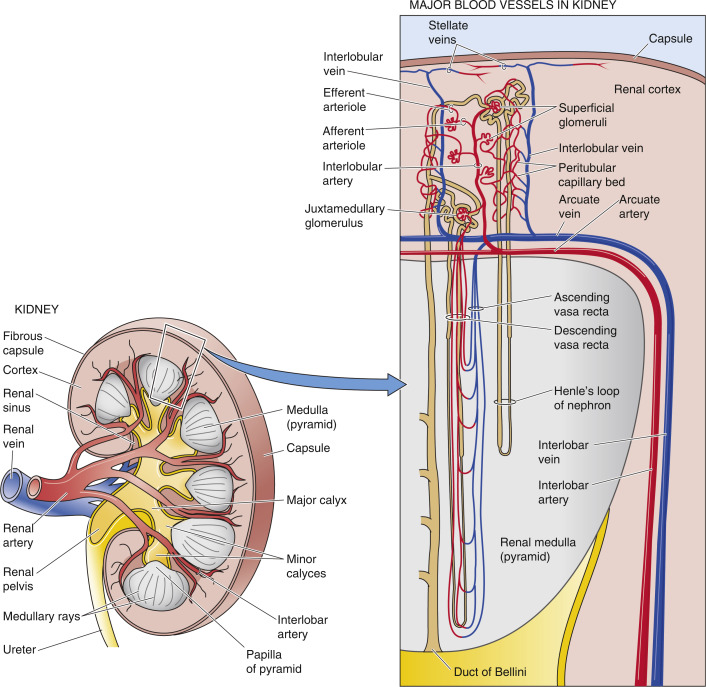
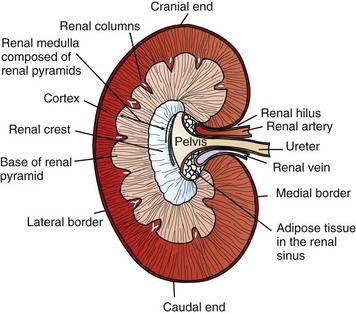
Causes of Ascending Vasa Recta Disorders
- Atherosclerosis: Hardening of the arteries due to plaque buildup.
- Hypertension: High blood pressure damaging blood vessels.
- Diabetes Mellitus: High blood sugar affecting blood vessel function.
- Renal Artery Stenosis: Narrowing of the renal artery.
- Thrombosis: Blood clots forming in the vasa recta.
- Embolism: Obstruction of blood flow by a clot or debris.
- Inflammatory Diseases: Conditions like vasculitis affecting blood vessels.
- Infections: Such as pyelonephritis leading to blood vessel issues.
- Autoimmune Disorders: Diseases where the body attacks its own tissues.
- Trauma: Injury to the kidneys affecting blood vessels.
- Smoking: Damaging blood vessels and reducing circulation.
- Obesity: Contributing to hypertension and diabetes.
- Chronic Kidney Disease: Long-term kidney damage.
- Age: Older age can increase risk factors.
- Genetic Disorders: Inherited conditions affecting blood vessels.
- Cholesterol Disorders: High levels affecting blood vessel health.
- Sedentary Lifestyle: Lack of exercise impacting circulation.
- Diet: High salt or fat intake affecting blood pressure.
- Alcohol Abuse: Damaging effects on blood vessels.
- Medications: Certain drugs affecting blood vessel integrity.
Symptoms of Ascending Vasa Recta Disorders
- High Blood Pressure: Elevated blood pressure readings.
- Kidney Pain: Discomfort or pain in the lower back.
- Swelling: In areas like legs and ankles due to fluid retention.
- Fatigue: Feeling unusually tired or weak.
- Urinary Changes: Changes in urine output or color.
- Nausea: Feeling sick or queasy.
- Vomiting: Expelling contents from the stomach.
- Headaches: Persistent or severe headaches.
- Dizziness: Feeling lightheaded or faint.
- Blurred Vision: Changes in vision clarity.
- Shortness of Breath: Difficulty in breathing.
- Chest Pain: Pain or discomfort in the chest area.
- Rapid Heart Rate: Increased heart rate or palpitations.
- Weight Gain: Sudden increase in weight due to fluid retention.
- Skin Changes: Rashes or unusual skin discoloration.
- Cramps: Muscle cramps or spasms.
- Fever: Elevated body temperature due to infection.
- Joint Pain: Discomfort in the joints.
- Increased Thirst: Persistent thirst.
- Anemia: Fatigue and weakness due to low red blood cells.
Diagnostic Tests
- Blood Tests: To check kidney function and electrolyte levels.
- Urine Tests: Analyzing urine for abnormalities.
- Imaging Studies: Ultrasound or CT scans to visualize blood flow.
- Angiography: Imaging of blood vessels using dye.
- Renal Biopsy: Taking a tissue sample for analysis.
- MRI: Magnetic resonance imaging for detailed images.
- Echocardiogram: Heart ultrasound to check overall heart function.
- X-rays: Imaging to rule out other conditions.
- Electrocardiogram (ECG): To assess heart rhythm.
- Blood Pressure Monitoring: Regular monitoring for hypertension.
- Vascular Studies: Assessing blood flow and vessel health.
- 24-hour Urine Collection: Measuring substances over a day.
- Kidney Function Tests: Assessing how well the kidneys are working.
- CT Angiography: Detailed imaging of blood vessels in the kidneys.
- Histological Examination: Microscopic examination of kidney tissue.
- Serum Creatinine: Blood test to assess kidney function.
- BUN Test: Blood urea nitrogen test for kidney health.
- Urinary Electrolytes: Checking electrolyte levels in urine.
- Cystoscopy: Direct visual examination of the bladder.
- Bone Marrow Test: In some cases, to rule out anemia causes.
Non-Pharmacological Treatments
- Diet Modification: Low salt and balanced diet.
- Weight Management: Maintaining a healthy weight.
- Exercise: Regular physical activity to improve circulation.
- Hydration: Drinking adequate fluids.
- Stress Management: Techniques like meditation and yoga.
- Smoking Cessation: Quitting smoking to improve health.
- Limit Alcohol: Reducing alcohol intake.
- Regular Check-Ups: Routine doctor visits to monitor health.
- Patient Education: Learning about the disorder.
- Sodium Restriction: Lowering sodium intake.
- Balanced Electrolyte Intake: Ensuring proper electrolyte balance.
- Adequate Sleep: Ensuring restful sleep for recovery.
- Physical Therapy: To strengthen muscles and improve function.
- Community Support: Joining support groups for emotional well-being.
- Biofeedback: Techniques to control physiological functions.
- Acupuncture: Alternative therapy for pain management.
- Massage Therapy: Reducing stress and promoting relaxation.
- Avoiding NSAIDs: Limiting non-steroidal anti-inflammatory drugs.
- Avoiding Over-the-Counter Cold Medicines: Some can affect blood pressure.
- Regular Blood Pressure Monitoring: Keeping track of blood pressure at home.
Medications
- ACE Inhibitors: For blood pressure control.
- Angiotensin II Receptor Blockers (ARBs): To manage hypertension.
- Diuretics: To reduce fluid retention.
- Statins: To manage cholesterol levels.
- Beta-blockers: To lower heart rate and blood pressure.
- Antibiotics: For infections related to the disorder.
- Antiplatelet Agents: To prevent blood clots.
- Anticoagulants: To manage blood clot risks.
- Corticosteroids: For inflammatory conditions.
- Immunosuppressants: For autoimmune disorders.
- Erythropoietin: For anemia management.
- Vasodilators: To widen blood vessels.
- Calcium Channel Blockers: For blood pressure control.
- Sodium Bicarbonate: For electrolyte balance.
- Phosphate Binders: For kidney-related phosphate issues.
- Calcium Supplements: For bone health in chronic kidney issues.
- Vitamin D: To support kidney health.
- Iron Supplements: For anemia.
- Pain Relievers: For managing discomfort.
- Nutritional Supplements: To ensure adequate nutrient intake.
Surgical Treatments
- Angioplasty: Widening narrowed blood vessels.
- Stenting: Inserting a device to keep vessels open.
- Renal Artery Bypass: Creating a bypass for blood flow.
- Nephrectomy: Removal of a kidney in severe cases.
- Vascular Reconstruction: Repairing damaged blood vessels.
- Embolectomy: Removing blood clots from vessels.
- Fistula Creation: For dialysis in chronic kidney disease.
- Transplantation: Kidney transplant for end-stage kidney failure.
- Surgery for Tumors: Removing tumors affecting blood flow.
- Aneurysm Repair: Fixing weakened blood vessels.
Prevention
- Healthy Diet: Eating nutritious foods.
- Regular Exercise: Staying physically active.
- Maintaining Healthy Weight: Managing weight through lifestyle.
- Monitoring Blood Pressure: Regular checks to manage hypertension.
- Controlling Blood Sugar: For diabetes management.
- Avoiding Tobacco: Quitting smoking.
- Limiting Alcohol: Reducing consumption.
- Staying Hydrated: Drinking enough water.
- Regular Medical Check-ups: Routine visits for early detection.
- Managing Stress: Using relaxation techniques.
When to See a Doctor
- If experiencing severe kidney pain.
- Persistent high blood pressure despite treatment.
- Sudden changes in urine output or color.
- Symptoms of infection (fever, chills).
- Unexplained fatigue or weakness.
- Sudden swelling in legs or ankles.
- Uncontrolled diabetes symptoms.
- New or worsening headaches.
- Any signs of chest pain or shortness of breath.
FAQs
Q1: What are ascending vasa recta disorders?
A1: They are conditions affecting the small blood vessels in the kidneys, impacting blood flow and kidney function.
Q2: What causes these disorders?
A2: They can be caused by conditions like hypertension, diabetes, and atherosclerosis.
Q3: How are they diagnosed?
A3: Through blood tests, urine tests, imaging studies, and sometimes biopsies.
Q4: What are the symptoms?
A4: Symptoms include high blood pressure, kidney pain, fatigue, and changes in urine.
Q5: Can these disorders be treated without medication?
A5: Yes, non-pharmacological treatments like diet changes and exercise can help.
Q6: What medications are commonly prescribed?
A6: ACE inhibitors, diuretics, and statins are often used.
Q7: Are there surgical options?
A7: Yes, surgeries like angioplasty and bypass can be performed in severe cases.
Q8: How can I prevent these disorders?
A8: Maintaining a healthy lifestyle, managing blood pressure, and regular check-ups are key.
Q9: When should I see a doctor?
A9: If you have severe kidney pain, high blood pressure, or other concerning symptoms.
Q10: Can lifestyle changes really make a difference?
A10: Yes, they can significantly improve health and reduce the risk of complications.
Q11: Is it possible to live a normal life with these disorders?
A11: Many people can manage their conditions effectively with treatment and lifestyle changes.
Q12: How often should I get my kidney function tested?
A12: Regular tests are recommended, especially if you have risk factors.
Q13: Are there specific diets for kidney health?
A13: Yes, diets low in salt and rich in fruits, vegetables, and whole grains are beneficial.
Q14: What is the role of hydration in kidney health?
A14: Staying hydrated helps maintain kidney function and prevents issues.
Q15: Can stress affect kidney health?
A15: Yes, chronic stress can impact overall health, including kidney function.
This outline serves as a starting point. You can expand each section with more details, examples, and data, while ensuring the language remains clear and accessible for readers
Disclaimer: Each person’s journey is unique, treatment plan, life style, food habit, hormonal condition, immune system, chronic disease condition, geological location, weather and previous medical history is also unique. So always seek the best advice from a qualified medical professional or health care provider before trying any treatments to ensure to find out the best plan for you. This guide is for general information and educational purposes only. Regular check-ups and awareness can help to manage and prevent complications associated with these diseases conditions. If you or someone are suffering from this disease condition bookmark this website or share with someone who might find it useful! Boost your knowledge and stay ahead in your health journey. We always try to ensure that the content is regularly updated to reflect the latest medical research and treatment options. Thank you for giving your valuable time to read the article.