Dry Eye Syndrome (also called Dry Eye Disease or DED) is a common condition where the front surface of the eye does not stay properly wet. Tears are needed to keep the eye surface smooth, clear, and healthy. In dry eye, either not enough tears are made, or the tears evaporate too quickly, or their quality is poor. This leads to irritation, discomfort, blurry vision, and sometimes damage to the eye surface. The core problem in dry eye is a cycle of tear film instability, surface damage, inflammation, and further tear dysfunction. This cycle is well described in the international TFOS DEWS reports, which are the global expert consensus on dry eye disease. TFOS Report ScienceDirect
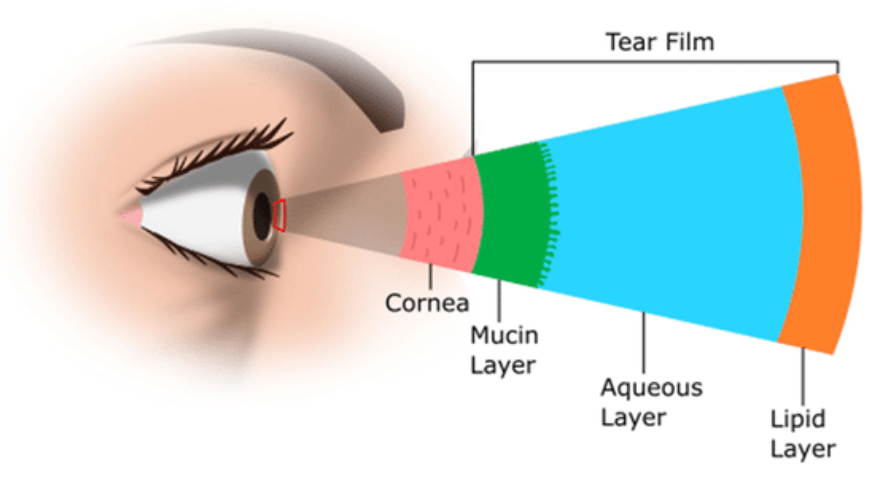
Dry Eye Syndrome (also called Dry Eye Disease or DED) is a common condition where the surface of the eye does not get enough good-quality tears to stay healthy and comfortable. It is not just “not enough water”—it is a problem of tear film instability, chronic inflammation, and loss of balance (homeostasis) on the eye’s surface. Tears normally lubricate, nourish, protect against infection, and keep vision clear. In dry eye, either the eyes don’t make enough tears (aqueous-deficient) or the tears evaporate too quickly because their oily layer is faulty (evaporative), or both. The instability leads to increased saltiness (hyperosmolarity), irritation, a cycle of surface inflammation, and sometimes damage to corneal cells. This modern, multifactorial understanding comes from large expert consensus efforts like TFOS DEWS II and the latest DEWS III updates, which define DED as a disease of the ocular surface with loss of tear film homeostasis, inflammation, and neurosensory abnormalities. tearfilm.orgTFOS ReportScienceDirect
There are three broad patterns: aqueous-deficient (tear production is low), evaporative (tear evaporation is too fast, often due to meibomian gland dysfunction), and mixed forms. In evaporative forms, the oily layer from meibomian glands is thickened or blocked; warm compresses and gland expression aim to correct that. Chronic inflammation of eyelid margins and ocular surface, often triggered by tear film saltiness and mechanical stress, further worsens symptoms. Neurosensory dysfunction—where the nerves sensing dryness become less effective or misfire—can also contribute. PMCTaylor & Francis OnlineTFOS Report
Types of Dry Eye Syndrome
Experts classify dry eye into main types based on what part of tear production or retention fails. The two broad categories are:
-
Aqueous Deficient Dry Eye (ADDE): This happens when the lacrimal glands (which produce the watery part of tears) do not make enough tear fluid. It can be due to autoimmune diseases (like Sjögren’s syndrome), aging, or damage to the glands. ScienceDirectPMC
-
Evaporative Dry Eye (EDE): Here, the tears evaporate too fast even if enough are made. The most common cause is dysfunction of the meibomian glands in the eyelids, which normally release oil that slows evaporation. Other contributors include poor blinking, eyelid position problems, and environmental conditions. NCBITFOS ReportScienceDirect
-
Mixed Dry Eye: Many patients have both reduced tear production and increased evaporation. In real life, dry eye often sits on a spectrum with overlap between aqueous-deficient and evaporative components. TFOS Report
-
Mucin Deficient Dry Eye: A lesser-emphasized subtype where the mucin layer (which helps tears stick to the eye) is abnormal because of reduced goblet cell function or surface disease. This impairs tear spreading and stability. PMC
-
Lipid Deficient / Meibomian Gland Dysfunction–related Dry Eye: Often embedded under evaporative causes, some classifications separate lipid-layer problems explicitly. Meibomian gland dropout, blockage, or altered secretion quality leads to a thin or poor oil layer and rapid tear loss. PMC
-
Neurotrophic / Neuropathic Dry Eye: When nerve sensing on the ocular surface is reduced or abnormal (for example after surgery or due to diabetes), the feedback loop that stimulates normal tear production and blinking is impaired. This can cause a mismatch between symptoms and signs. PMC
-
Contact Lens–Associated Dry Eye: The presence of a lens alters tear film dynamics and may mechanically disrupt tear spreading, leading to symptoms even if tear production is relatively normal. NCBI
-
Medication-Induced / Secondary Dry Eye: Certain drugs reduce tear production or change tear quality (see causes below). Mayo Clinic
These types help clinicians tailor diagnosis and treatment; the TFOS DEWS III update continues refining how these forms are identified and managed in practice. AjoScienceDirect
Causes of Dry Eye Syndrome
-
Aging: Tear production naturally decreases with age, and eyelid structures can change, contributing to both deficient production and increased evaporation. NCBI
-
Meibomian Gland Dysfunction (MGD): Blocked or poorly functioning oil glands cause a weak lipid layer, so tears evaporate quickly. MGD is the leading cause of evaporative dry eye. TFOS Report
-
Autoimmune Diseases (e.g., Sjögren’s Syndrome): These conditions attack glands that make tears (and saliva), especially in primary or secondary Sjögren’s, leading to marked aqueous deficiency. PMCMayo Clinic
-
Rheumatoid Arthritis / Lupus / Other Systemic Inflammatory Diseases: These can be associated with secondary Sjögren’s or independently cause ocular surface inflammation and tear instability. PMCMayo Clinic
-
Hormonal Changes: Changes in hormones, such as in menopause, can reduce tear production or change tear composition, increasing risk. Mayo Clinic
-
Environmental Factors: Dry air, wind, smoke, air conditioning, and heated indoor environments accelerate tear evaporation. NCBIeverett-hurite.com
-
Prolonged Visual Tasking / Screen Use: Looking at screens reduces blink rate and can cause incomplete blinking, leading to decreased tear spread and local drying. PMC
-
Contact Lens Wear: Lenses disrupt tear film and can cause mechanical irritation or alter tear dynamics, worsening dryness. NCBI
-
Vitamin A Deficiency: This affects the health of the ocular surface cells and goblet cells, impairing mucin production and tear film stability. NCBI
-
Blepharitis / Eyelid Inflammation: Chronic eyelid margin inflammation, often with bacterial overgrowth or Demodex mites, disrupts meibomian gland function and tear quality.
-
Eyelid Position Abnormalities (e.g., Lagophthalmos): If the eyelids do not close completely, the surface stays exposed and tears evaporate.
-
Recent Ocular Surgery (e.g., LASIK): Surgery can damage corneal nerves and reduce tear reflexes, sometimes causing transient or chronic dry eye.
-
Medications: Many medicines lower tear production or alter tear composition. Common examples include antihistamines, decongestants, antidepressants, beta-blockers, diuretics, and some acne medications. Mayo Clinic
-
Systemic Diseases (Diabetes, Thyroid Disease): Diabetes can damage corneal nerves and worsen tear production; thyroid eye disease may affect eyelid function and surface exposure. NCBI
-
Allergic Eye Disease: Chronic allergy can inflate surface inflammation and disrupt tear film integrity, sometimes with reflex tearing that masks underlying dryness. PMC
-
Reduced Goblet Cell Density: Injury, inflammation, or surgery can lower goblet cell numbers, decreasing mucin and destabilizing the tear film.
-
Cranial Nerve / Neurological Injury: Damage that impairs corneal sensation or blink reflex (e.g., after stroke or nerve palsy) can disrupt normal protective mechanisms. PMC
-
Chronic Inflammation of the Ocular Surface: Persistent surface inflammation (from any source) perpetuates tear film breakdown and reduces tear quality. Frontiers
-
Preservatives in Eye Drops (e.g., Benzalkonium Chloride): Long-term use of preserved drops can harm surface cells and contribute to dry eye. Frontiers
-
Contact with Irritants or Chemical Exposure: Occupational exposures (e.g., fumes, pollutants) can directly irritate the ocular surface and accelerate tear evaporation. PMC
Symptoms of Dry Eye Syndrome
Dry eye symptoms can vary in severity and may not always match the clinical signs. Common complaints include:
-
Eye Dryness Feeling: A sensation that the eye is dry or “not wet enough.” PMC
-
Burning or Stinging: A sharp, uncomfortable feeling, often worse in dry environments. PMC
-
Foreign Body Sensation: Feeling like there is something gritty or sandy in the eye. PMC
-
Redness: Mild to moderate redness from irritation and inflammation. PMC
-
Light Sensitivity (Photophobia): Eyes become more sensitive to bright lights. PMC
-
Blurred or Fluctuating Vision: Vision that gets blurry, especially during tasks like reading, due to unstable tear film. PMC
-
Excess Tearing (Reflex): Ironically, dry eye can cause watery eyes because irritation triggers reflex tear production. PMC
-
Eye Fatigue or Tired Eyes: Eyes feel tired after short periods of work, especially reading or screen time. PMC
-
Stringy Mucus in or around the Eyes: Thick discharge, especially in more chronic or inflammatory forms. PMC
-
Difficulty Wearing Contact Lenses: Discomfort or intolerance, often due to tear film instability. NCBI
-
Itching: May overlap with allergy but can be a dry eye symptom from surface irritation. PMC
-
Soreness or Aching: General discomfort of the eyes, sometimes described as a dull ache. PMC
-
Difficulty with Night Driving: Glare and halos from tear film irregularity make vision harder in low light. PMC
-
Sensitivity to Wind or Air Movement: Wind causes more immediate discomfort due to rapid tear loss. PMC
-
Increased Blink or Incomplete Blink Awareness: Patients may feel they are blinking more or not fully, affecting tear spread. PMC
Diagnostic Tests for Dry Eye Syndrome
Diagnosis combines symptoms and objective testing. The TFOS DEWS protocols recommend a stepwise approach using both simple and advanced tests to identify the subtype and severity. AjoScienceDirect
A. Physical Exam (basic in-office observation)
-
Eyelid Margin Inspection: Doctor looks at the eyelid edges for redness, swelling, and abnormal gland openings (signs of blepharitis or MGD). EyeWiki
-
Blink Rate and Completeness Check: Watching how often and fully the patient blinks, since low or incomplete blinking worsens dry eye. PMC
-
Tear Meniscus Height Assessment: Visual estimate of the thin strip of tear fluid along the lower eyelid; low height suggests low tear volume. EyeWiki
-
Slit-Lamp Biomicroscopy: Using a microscope to examine the cornea, conjunctiva, and tear film for signs of damage, inflammation, and debris. EyeWiki
-
Conjunctival and Corneal Staining (Fluorescein / Lissamine Green): Dyes applied to show damaged cells or areas of poor tear coverage; important to grade surface injury. PMCThe Open Ophthalmology Journal
B. Manual Functional Tests
-
Schirmer Test I (without anesthesia): Measures basic plus reflex tear production by placing filter paper strips under lower eyelid and seeing how much wets in 5 minutes. EyeWiki
-
Schirmer Test II (with nasal stimulation or with anesthesia variant): Separates reflex from basal tear production; often used when more nuance is needed. EyeWiki
-
Tear Breakup Time (TBUT): After instilling fluorescein dye, time is measured until dry spots appear on the tear film; short breakup time means unstable tears. EyeWiki
-
Meibomian Gland Expression / Pressure: Gentle pressure on the eyelid to see quality and quantity of the oil released from meibomian glands; poor secretion supports evaporative dry eye. EyeWiki
-
Corneal Esthesiometry (Cochet-Bonnet or Similar): Tests corneal sensation (nerve function) because decreased sensitivity can hide symptoms or reflect neuropathic components. PMC
C. Lab and Pathological Tests
-
Tear Osmolarity Measurement: High tear salt concentration (osmolarity) is a hallmark of dry eye; point-of-care devices quantify this to help confirm diagnosis. Frontiers
-
MMP-9 Inflammation Test (InflammaDry): Detects matrix metalloproteinase-9, a marker of ocular surface inflammation; elevated levels support inflammatory dry eye. PMCFrontiers
-
Autoantibody Panel for Sjögren’s (Anti-SSA/Ro, Anti-SSB/La): Blood tests check for antibodies linked to Sjögren’s syndrome when aqueous deficiency is suspected. PMC
-
Rheumatoid Factor / ANA / Other Systemic Markers: To screen for associated autoimmune diseases in appropriate clinical contexts. PMC
-
Thyroid Function Tests: Thyroid disease can affect ocular surface and eyelid function, increasing dry eye risk. NCBI
-
Blood Glucose / HbA1c: Diabetes can reduce corneal nerve function and contribute to dry eye; testing helps identify systemic contributors. NCBI
-
Vitamin A Level: Low vitamin A can impair surface cell health and mucin production, so deficiency evaluation can be useful in certain settings. NCBI
-
Microbiologic Culture or PCR (for chronic blepharitis or infection): If infection or overgrowth is suspected to be driving inflammation and tear film disruption. PMC
D. Electrodiagnostic / Specialized Functional Tests
-
Tear Clearance / Tear Dynamics Testing: Using fluorescein or other tracers to see how tears flow and drain, which can be delayed in some functional disorders (overlaps with tear film stability evaluation). EyeWiki
-
Lacrimal Gland Function Imaging (e.g., Dacryoscintigraphy): Nuclear medicine test to measure tear drainage and lacrimal system flow; helps if drainage or production abnormalities are suspected. (This blends functional evaluation with imaging.) Ajo
E. Imaging Tests (some overlap with above but focused on structure)
(Note: Though user asked for categorization, many modern exams combine imaging with functional data; the next few are often used to visualize structures.)
-
Meibography (Infrared Imaging of Meibomian Glands): Shows gland dropout, dilation, and structural loss; critical to assess MGD severity. EyeWiki
-
Anterior Segment Optical Coherence Tomography (AS-OCT): Measures tear meniscus height, evaluates eyelid–ocular surface relationships, and quantifies tear volume. EyeWiki
-
In Vivo Confocal Microscopy: Allows high-resolution imaging of corneal nerves and cells, useful in neuropathic or severe surface disease. Frontiers
-
Interferometry (Lipid Layer Thickness): Noninvasive measurement of the tear film’s oil layer to identify evaporative components. EyeWiki
-
Ocular Surface Thermography: Detects temperature changes across the eye’s surface as a marker of inflammation or tear film instability. Frontiers
Non-Pharmacological Treatments
-
Warm Compresses: Applying a warm compress to the eyelids softens thickened meibum in the meibomian glands, helping it flow and restore the oily tear layer. Regular use (once or twice daily for 5–10 minutes) melts abnormal secretions and reduces evaporative dry eye. PMCTaylor & Francis Online
-
Eyelid Hygiene / Lid Scrubs: Cleaning eyelid margins with mild lid scrubs removes debris, bacteria, and biofilm that worsen inflammation. This reduces blepharitis and supports gland function, improving tear quality. Taylor & Francis OnlineThe Journal of Medical Optometry (JoMO)
-
Tea Tree Oil for Demodex Blepharitis: Demodex mites on eyelash follicles can inflame eyelids; controlled use of tea tree oil products (usually in-office or diluted at home) targets these mites, reducing blepharitis and secondary dry eye. Use cautiously to avoid irritation. PMCAJMC
-
Blinking Exercises: Many people under-blink or have incomplete blinks, reducing tear spread and renewal. Guided blinking exercises (e.g., conscious full blinks multiple times per hour) improve tear film stability and symptoms. Apps or routines can optimize frequency. ScienceDirectPubMedScienceDirect
-
Environmental Humidifiers: Adding moisture to dry air (especially in air-conditioned or heated indoor spaces) reduces tear evaporation, helping maintain tear film integrity. Humidifiers are especially useful in winter or low-humidity climates. TFOS Report
-
Avoiding Air Drafts and Wind Exposure: Direct airflow from fans, car vents, or windy environments increases tear evaporation. Simple behavioral adjustments like shielding eyes or reducing direct drafts help protect the tear film. ScienceDirect
-
Screen Breaks and Ergonomics (20-20-20 Rule): Staring at screens reduces blink rate. Breaking every 20 minutes to look 20 feet away for 20 seconds encourages natural blinking and reduces ocular surface stress. Position screens slightly below eye level to minimize ocular surface exposure. ScienceDirect
-
Scleral Lenses: These specialized contact lenses vault over the cornea, trapping a reservoir of fluid that continuously bathes and protects the ocular surface, beneficial in severe or refractory dry eye. They also shield the eye from evaporation and friction. PMCPMCPentaVision
-
Moisture Chamber Goggles: Wearing moisture goggles, especially during sleep or in very dry settings, creates a humid microenvironment around the eyes to prevent tear evaporation. Useful temporary protection without medication. ScienceDirect
-
Thermal Pulsation Systems (e.g., LipiFlow): These in-office devices apply heat and gentle pressure to meibomian glands to unclog them, restoring lipid flow and improving evaporative dry eye. The combination of sustained heat and expression targets underlying gland obstruction. PMC
-
Intense Pulsed Light (IPL): IPL applied around eyelids reduces abnormal blood vessel growth, decreases inflammation, and may improve meibomian gland function, leading to better tear stability. Multiple sessions show symptomatic and clinical improvements. Wiley Online Library
-
TearCare and Similar Localized Eyelid Heating/Expression: Systems like TearCare deliver targeted heat to lids while allowing the patient to blink, followed by gland expression, combining thermal therapy with mechanical clearance. PMC
-
Manual Meibomian Gland Expression: Performed by clinicians to physically clear blocked glands, often following warm compresses to soften secretions. Helps restore the lipid layer. Taylor & Francis Online
-
Allergen Control: For allergy-associated dry eye, reducing exposure to dust mites, pet dander, pollen, and indoor molds decreases ocular surface inflammation and secondary dryness. ScienceDirect
-
Smoking Cessation and Air Pollution Avoidance: Tobacco smoke and airborne pollutants irritate the ocular surface, worsen tear quality, and promote inflammation; quitting smoking and avoiding polluted environments helps preserve tear film health. ScienceDirect
-
Hydration and Lifestyle: Adequate systemic hydration supports tear production. Avoiding excessive caffeine or alcohol that can dehydrate and using lifestyle measures to maintain general vascular health helps the ocular surface indirectly. ScienceDirect
-
Protective Eyewear / Sunglasses: Wearing wraparound sunglasses outdoors or in windy situations protects against evaporative stress and UV-related ocular surface inflammation. ScienceDirect
-
Optimizing Sleep and Eyelid Position: Poor sleep or eyelid malposition during rest (e.g., incomplete closure) can cause exposure-related dryness. Addressing sleep quality and, if necessary, using eye shields can mitigate this. NYU Langone Health
-
Reducing Contact Lens Wear or Improving Lens Hygiene: Contact lenses can disrupt tear film; cutting back wear time or improving lens cleaning reduces induced dryness and irritation. ScienceDirect
-
Stress Reduction and General Anti-inflammatory Lifestyle: Chronic stress can worsen systemic inflammation and ocular surface sensitivity. Mindfulness, regular moderate exercise, and managing systemic inflammatory conditions help support tear film homeostasis. ScienceDirect
Drug Treatments
-
Preservative-Free Artificial Tears (Lubricant Eye Drops): These are over-the-counter viscous solutions (e.g., carboxymethylcellulose, hyaluronic acid, polyethylene glycol) used many times daily to supplement the tear film. They lubricate the eye, dilute inflammatory mediators, and temporarily improve comfort. Use as needed; frequency can be 4–8 times/day or more in severe dryness. Side effects are minimal; some formulas cause transient blurring. TFOS ReportScienceDirect
-
Cyclosporine Ophthalmic Emulsion (e.g., Restasis, Cequa): Class: Calcineurin inhibitor / immunomodulator. Dosage: One drop in each affected eye twice daily (approximately every 12 hours). Purpose: Reduce ocular surface inflammation and increase tear production over weeks to months. Mechanism: Inhibits T-cell activation and inflammatory cytokine release, restoring lacrimal gland function. Side effects: Burning/stinging on instillation, redness, blurred vision, rare hypersensitivity. Mayo ClinicMedlinePlusCleveland ClinicDrugs.comCleveland Clinic
-
Lifitegrast Ophthalmic Solution 5%: Class: Lymphocyte function-associated antigen-1 (LFA-1) antagonist. Dosage: One drop in each eye twice daily. Purpose: Treat signs and symptoms of dry eye by reducing inflammation. Mechanism: Blocks interaction between LFA-1 and ICAM-1, reducing T-cell mediated inflammation on ocular surface. Side effects: Eye irritation, dysgeusia (altered taste), blurred vision, punctate keratitis. PMCPMCWiley Online LibraryLippincott JournalsSpringerLinkDrugBank
-
Topical Corticosteroids (e.g., Loteprednol 0.5%): Class: Anti-inflammatory steroid. Dosage: Short courses, typically 1–2 drops 2–4 times daily for 1–2 weeks, then tapered under ophthalmologist guidance. Purpose: Calm acute surface inflammation and flare-ups. Mechanism: Broad suppression of inflammatory cytokines and immune cell activity. Side effects (with prolonged use): Elevated intraocular pressure, cataract formation; hence limited to short-term under supervision. TFOS ReportScienceDirect
-
Topical Azithromycin (e.g., Azithromycin in DuraSite): Class: Macrolide antibiotic / anti-inflammatory. Dosage: Typically one drop twice daily for several days, then once daily for a total course as directed. Purpose: Improve meibomian gland function and reduce eyelid margin inflammation in MGD-related dry eye. Mechanism: Antimicrobial action plus modulation of lipid composition and anti-inflammatory effects on eyelid glands. Side effects: Mild irritation, blurred vision. PMCPMC
-
Oral Doxycycline: Class: Tetracycline antibiotic with anti-inflammatory properties. Dosage: 100 mg once or twice daily (often 100 mg daily) for 4–6 weeks (low-dose regimens can be used long-term in some patients). Purpose: Treat evaporative dry eye caused by meibomian gland dysfunction by reducing inflammation and altering meibum composition. Mechanism: Inhibits matrix metalloproteinases, reduces bacterial lipases, anti-inflammatory effects. Side effects: Photosensitivity, gastrointestinal upset, potential esophageal irritation; avoid in pregnancy/children (teeth discoloration). ScienceDirectWiley Online Library
-
Oral Azithromycin (Pulse Therapy): Class: Macrolide antibiotic. Dosage: Example regimen: 1 g once weekly for 3 weeks. Purpose: Alternative for MGD inflammation when doxycycline is not tolerated. Mechanism: Anti-inflammatory effects and alteration of microbial flora on eyelid margin. Side effects: Gastrointestinal upset, rare cardiac conduction effects. JAMA Network
-
Mucin Secretagogues (e.g., Rebamipide Ophthalmic Suspension or Diquafosol): Class: Tear film enhancers / mucin promoters. Dosage: Varies by agent—rebamipide often used as 2% ophthalmic suspension several times daily; diquafosol is typically 3% solution four times daily. Purpose: Improve tear film stability by increasing mucin production. Mechanism: Stimulates goblet cells to secrete mucins and enhances epithelial function, reducing tear breakup. Side effects: Mild irritation, rare allergic reactions. NaturePMCPubMedScienceDirectIOVS
-
Oral Pilocarpine: Class: Muscarinic agonist / secretagogue. Dosage: 5 mg three times daily (dose adjusted for tolerance). Purpose: Stimulate exocrine (including lacrimal) secretion in systemic conditions like Sjögren’s syndrome with dry eye and mouth. Mechanism: Activates muscarinic receptors to increase tear and saliva production. Side effects: Sweating, gastrointestinal upset, urinary frequency, bronchospasm (caution in asthma). ScienceDirect
-
Oral Cevimeline: Class: Muscarinic agonist (M3 receptor selective). Dosage: 30 mg three times daily. Purpose: Similar to pilocarpine for Sjögren’s-associated aqueous deficiency. Mechanism: Stimulates exocrine gland secretion via muscarinic receptor activation. Side effects: Sweating, gastrointestinal disturbances, increased urinary frequency. ScienceDirect
Dietary Molecular Supplements
-
Omega-3 Fatty Acids (EPA/DHA): Typical Dosage: 1000 mg of combined EPA/DHA twice daily. Function: Anti-inflammatory support for the ocular surface. Mechanism: Converts to less inflammatory eicosanoids, reduces ocular surface inflammation, and may improve meibomian gland secretions. Evidence is mixed but many guidelines include omega-3 for chronic dry eye. PMCNCCIH
-
Vitamin A (as Retinol or Beta-Carotene): Dosage: From diet (carrots, sweet potatoes) or low-dose supplements; avoid high-dose preformed vitamin A due to toxicity. Function: Maintains healthy conjunctival and corneal epithelium. Mechanism: Supports mucin production and epithelial cell differentiation; deficiency leads to ocular surface keratinization and dryness. Healthline
-
Vitamin D: Dosage: 1000–2000 IU daily (adjust if deficient based on blood levels). Function: Modulates inflammation. Mechanism: Vitamin D receptors on ocular surface cells help regulate immune response and reduce inflammatory cytokines in dry eye. Healthline
-
Vitamin B12: Dosage: Typically 500–1000 mcg orally daily or injectable for deficiency. Function: Nerve health and ocular surface comfort. Mechanism: May help neurosensory components of dry eye by supporting corneal nerve integrity, reducing neuropathic pain features. Healthline
-
Vitamin C: Dosage: 500 mg twice daily. Function: Antioxidant protection for ocular surface cells. Mechanism: Scavenges oxidative stress, which contributes to inflammation and epithelial damage in dry eye. Prevention
-
Zinc: Dosage: 15–25 mg daily (avoid excessive doses). Function: Supports tissue repair and antioxidant enzyme systems. Mechanism: Cofactor for many enzymes involved in ocular surface homeostasis and immune regulation. Prevention
-
Curcumin (with Piperine): Dosage: Varies; typical bioavailable formulations provide 500 mg curcumin with piperine once or twice daily. Function: Anti-inflammatory. Mechanism: Inhibits NF-kB and reduces pro-inflammatory cytokines, potentially easing ocular surface inflammation. Prevention
-
Green Tea Extract (EGCG): Dosage: Equivalent of 1–2 cups/day or standardized supplement. Function: Anti-oxidative and mild anti-inflammatory. Mechanism: Epigallocatechin gallate reduces inflammation and oxidative damage on the ocular surface. Prevention
-
N-acetylcysteine (NAC): Dosage: 600 mg once or twice daily (oral) or topical formulations in research use. Function: Improves mucin quality and reduces surface inflammation. Mechanism: Precursor to glutathione, reduces oxidative stress, may break abnormal mucous crosslinks improving tear film. ScienceDirect
-
Oral Hyaluronic Acid: Dosage: Varies by product (often 120–240 mg daily). Function: Systemic support for hydration and possibly tear film stability (emerging evidence). Mechanism: May improve mucosal hydration and ocular surface comfort via systemic effects; evidence is limited and evolving. ScienceDirect
Advanced Regenerative / Immune-Modulating Therapies
-
Autologous Serum Eye Drops: These are made from the patient’s own blood, diluted (often 20%) and used as tears. Purpose: Provide epitheliotrophic growth factors, vitamins, and proteins that mimic natural tears and promote healing. Mechanism: Contains EGF, fibronectin, vitamin A, and others that aid epithelial repair and reduce inflammation. Used in severe or refractory dry eye, especially aqueous-deficient types. PMCPMCAAO JournalFrontiers
-
Platelet-Rich Plasma (PRP) Eye Drops: Similar to serum but richer in growth factors; often used for severe ocular surface disease. Purpose: Accelerate healing, reduce inflammation, and improve tear film. Mechanism: High concentrations of platelet-derived growth factors restore epithelial integrity and modulate immune response. Studies show comparable or sometimes superior outcomes to serum in certain patients. NaturePMCbmjophth.bmj.comLippincott Journals
-
Amniotic Membrane Therapy (e.g., PROKERA): Class: Biologic scaffold applied to the ocular surface. Purpose: Promote healing and reduce inflammation in severe surface disease. Mechanism: Amniotic membrane delivers anti-scarring, anti-inflammatory factors and supports epithelial regeneration when placed on the eye. NYU Langone Health
-
Mesenchymal Stem Cell (MSC)–Derived Exosomes / MSC-Based Therapy: Purpose: Modulate inflammation and promote tissue repair in refractory dry eye. Mechanism: Exosomes from MSCs carry anti-inflammatory cytokines and regulatory signals, suppressing pathogenic immune cells and enhancing epithelial recovery. Early human and animal studies show decreased surface inflammation and improved signs. PMCPMCScienceDirectMDPI
-
Recombinant Human Nerve Growth Factor (Cenegermin): Originally approved for neurotrophic keratitis, it fosters corneal nerve and epithelial regeneration, which can indirectly benefit dry eye by restoring normal sensation and trophic support. Dosage: Typically 0.002% eye drops (per approved regimen) administered multiple times daily for 8 weeks under specialist care. Mechanism: Binds TrkA receptors to support nerve health and epithelial healing. PMCPMCAAO Journalbjo.bmj.com
-
Systemic or Topical Mesenchymal Stem Cell Therapy (Experimental/In Development): Direct use of MSCs (e.g., ocular surface injections or eye drops) is under investigation for severe DED. Purpose: Immune regulation and regeneration of lacrimal and ocular surface tissue. Mechanism: MSCs secrete anti-inflammatory factors, induce regulatory T cells, and may restore glandular function. Early trials show promising improvements in tear production and inflammation. BioMed CentralScienceDirectWJGNet
Surgical / Procedural Interventions
-
Punctal Occlusion (Plugs or Cautery): Small devices (temporary or permanent) are placed in the tear drainage openings (puncta) to block tear outflow, conserving natural tears. Cauterization can permanently close puncta if plugs help. Used when tear production is insufficient but tear drainage is too rapid. AAONYU Langone HealthPubMed
-
Meibomian Gland Probing / Expression: In-office mechanical opening of blocked meibomian gland orifices, often after heating, releases trapped meibum and restores lipid layer flow. It’s done to relieve obstruction in evaporative dry eye. Taylor & Francis Online
-
Tarsorrhaphy (Partial Eyelid Closure): Surgical narrowing of the eyelid opening to reduce ocular surface exposure, especially in severe dry eye with exposure keratopathy or poor eyelid closure. It protects the cornea from drying and promotes healing. NYU Langone Health
-
Amniotic Membrane Transplantation: Placement of preserved amniotic membrane on the ocular surface surgically to reduce inflammation and promote epithelial regeneration in severe or non-healing cases. AAO Journal
-
Eyelid Malposition Correction (Ectropion/Entropion Repair): Surgical correction of eyelid position that causes abnormal exposure or eyelash contact, which worsens dryness and irritation. Restoring normal eyelid anatomy reduces mechanical stress and tear film disruption. NYU Langone Health
Key Prevention Strategies
To reduce risk or progression of dry eye, patients should: maintain regular eyelid hygiene, limit prolonged screen time and use blinking reminders, protect eyes from wind and low humidity with eyewear or humidifiers, avoid smoking and pollution, stay well hydrated, manage underlying inflammation (e.g., treat blepharitis early), ensure adequate dietary omega-3 and antioxidants, control systemic diseases like autoimmune disorders, avoid overuse of contact lenses, and review medications that may dry eyes with a doctor. Early identification and treatment of meibomian gland dysfunction also prevents chronicity. PMCScienceDirect
Diet: What to Eat and What to Avoid
Eat (Support Eye Surface Health): Include oily fish (salmon, mackerel) for omega-3s; leafy greens, eggs, and carrots for lutein, zeaxanthin, and vitamin A; citrus fruits for vitamin C; nuts and seeds for vitamin E and zinc; fortified dairy or fatty fish for vitamin D; whole grains and anti-inflammatory spices like turmeric (curcumin) to reduce systemic inflammation; adequate water to maintain hydration; and probiotic-containing foods to support systemic immune balance. PreventionHealthline
Avoid (Things That Worsen Dry Eye): Excessive caffeine or alcohol that can cause dehydration; high-sodium processed foods that worsen fluid imbalance; trans fats and diets with very high omega-6 to omega-3 ratios which propagate inflammation; smoking and exposure to secondhand smoke; allergenic triggers if sensitive; prolonged unbroken screen viewing; and environmental irritants such as dust or chemical fumes. ScienceDirect
When to See a Doctor
You should see an eye doctor if you have severe, persistent eye dryness not improving with basic home care, sudden vision changes, intense eye pain, light sensitivity, a feeling of a foreign body that doesn’t go away, discharge or crusting suggestive of infection, inability to open the eye easily, worsening with systemic autoimmune disease, or signs of surface damage (such as persistent redness or corneal staining). If over-the-counter drops and lifestyle modifications fail after 1–2 weeks or symptoms significantly interfere with daily life, professional evaluation is warranted. TFOS ReportScienceDirect
Frequently Asked Questions (FAQs)
-
What causes dry eye syndrome?
Dry eye is caused by poor tear production, fast tear evaporation (often from meibomian gland dysfunction), inflammation, or combinations of these. Age, hormones, environment, medications, and autoimmune diseases like Sjögren’s contribute. ScienceDirectPMC -
Is dry eye permanent?
It can be chronic, but many people manage or improve it with proper treatment. Some underlying causes (like meibomian dysfunction) can be treated to reduce symptoms long-term. TFOS ReportTaylor & Francis Online -
Are artificial tears enough?
For mild to moderate cases, preservative-free artificial tears often suffice. Persistent or inflammatory dry eye usually needs anti-inflammatory therapy (e.g., cyclosporine or lifitegrast). Mayo ClinicPMC -
How long before prescription drops work?
Immunomodulators like cyclosporine or lifitegrast can take 4–12 weeks to show full benefit, though some symptom relief may begin earlier. PMCWiley Online Library -
Can diet help dry eye?
Yes. Increasing omega-3 intake, antioxidants, and staying hydrated supports tear film health and reduces inflammation. Avoiding pro-inflammatory foods and dehydration triggers also helps. PMCPrevention -
Are there side effects of common dry eye drugs?
Yes. Cyclosporine may burn briefly, lifitegrast can cause altered taste, steroids (if overused) can raise eye pressure, and antibiotics have their own systemic profiles. Most side effects are mild and manageable. Mayo ClinicPMC -
What is the role of omega-3 supplements?
They reduce inflammation and may improve tear quality, though results vary between individuals. Quality and dose matter. NCCIH -
When are serum or PRP drops used?
In moderate to severe or refractory dry eye, especially when standard treatments fail, because they supply growth factors and healing components similar to natural tears. PMCPMC -
Can dry eye cause vision loss?
Severe untreated dry eye can damage the corneal surface, leading to scarring or infection, which may affect vision. Early treatment prevents complications. TFOS Report -
Is screen time making it worse?
Yes. Reduced blink rate during screen use leads to tear film breakup; regular breaks and conscious blinking help. ScienceDirect -
Can eyelid problems cause dry eye?
Yes. Malpositions like ectropion or entropion and blepharitis disrupt tear distribution or cause surface irritation; correcting them improves dry eye. NYU Langone Health -
What’s the difference between evaporative and aqueous-deficient dry eye?
Evaporative is due to a poor lipid layer (often meibomian gland dysfunction), leading to fast tear loss; aqueous-deficient is due to low volume from lacrimal gland insufficiency (e.g., Sjögren’s). Many patients have both. ScienceDirect -
Are surgeries common?
Only in moderate to severe cases or when anatomy contributes (e.g., punctal occlusion, tarsorrhaphy, eyelid correction). Most people are managed medically first. AAONYU Langone Health -
Can inflammation be fully controlled?
Often yes, with consistent use of anti-inflammatory agents and addressing underlying contributors. Some chronic cases flare and need ongoing management. PMCPMC -
Is dry eye a sign of systemic disease?
Yes. Conditions like Sjögren’s syndrome, rheumatoid arthritis, and thyroid disorders can present with dry eye, so persistent or severe symptoms may prompt systemic evaluation. ScienceDirect
Disclaimer: Each person’s journey is unique, treatment plan, life style, food habit, hormonal condition, immune system, chronic disease condition, geological location, weather and previous medical history is also unique. So always seek the best advice from a qualified medical professional or health care provider before trying any treatments to ensure to find out the best plan for you. This guide is for general information and educational purposes only. Regular check-ups and awareness can help to manage and prevent complications associated with these diseases conditions. If you or someone are suffering from this disease condition bookmark this website or share with someone who might find it useful! Boost your knowledge and stay ahead in your health journey. We always try to ensure that the content is regularly updated to reflect the latest medical research and treatment options. Thank you for giving your valuable time to read the article.
The article is written by Team RxHarun and reviewed by the Rx Editorial Board Members
Last Updated: August 02, 2025.



